Contents [Back to main page] [CGD home] [About CGD]
- [top]
- 1. Disease Burden and the New Bottom Billion
- 2. Recommendations
- Eliminate country-income thresholds or classifications as across-the-board eligibility criteria for global health funding
- Set up regional pooled procurement schemes or negotiate an LMIC public-sector price within existing procurement mechanisms
- Build evidence-based priority-setting institutions in middle-income countries
- Establish increased accountability mechanisms and providing technical support to MICs
- 3. Going Forward
Global Health and the New Bottom Billion: How Funders Should Respond to Shifts in Global Poverty and Disease Burden
Amanda Glassman, Denizhan Duran, and Andy Sumner
January 2012
After a decade of rapid economic growth, many developing countries have attained middle-income-country (MIC) status. But poverty reduction in these countries has not kept pace with economic growth. As a result, most of the world's poor-up to a billion people-now live in these new MICs, making up a “new bottom billion.” As the new MICs are home to most of the world's poor, they also carry the majority of the global disease burden. This poses a challenge to global health agencies, in particular GAVI and the Global Fund, which are accustomed to disbursing funds on the assumption that the majority of poor people live in poor countries.
To better target aid to poor people, we recommend that funders focus on four areas:
- Eliminating country-income thresholds as across-the-board criteria for allocating global health funding.
- Setting up regional pooled procurement or pricing mechanisms.
- Building evidence-based priority-setting institutions.
- Establish increased accountability mechanisms and providing technical support for MICs.
Over the past decade, 28 countries graduated from low-income status to middle-income status because of rapid economic growth. While the number of low-income countries (LICs) will continue to fall drastically in the coming years, [1] the number of people living in poverty has remained fairly steady, if China is excluded. As a result, over 70 percent of the world's poor have “moved" into middle-income countries (MICs) simply by way of their countries' graduating from low-income status. An estimated 960 million of the world's poorest people—a “new bottom billion”—live in MICs that, despite impressive growth rates, trap millions in extreme poverty as a result of inequality and demographic trends. [2]
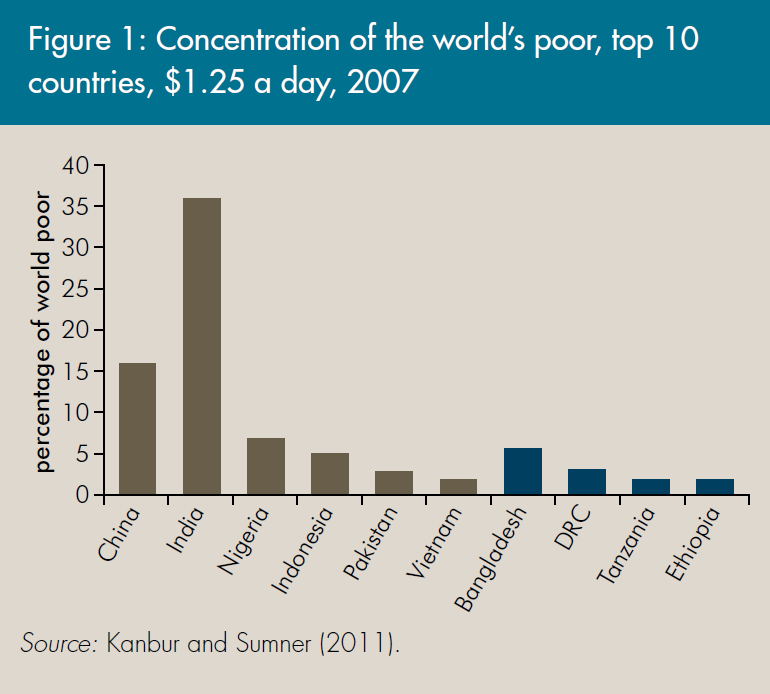
This shift is due in part to a high concentration of the world's poor in relatively few countries. About 60 percent of the world's poor live in just five populous new MICs: Pakistan, India, Nigeria, China, and Indonesia-the “big 5,” or PINCI. Indeed, of the top 10 countries by contribution to global poverty, only four are LICs-Bangladesh, DRC, Tanzania, and Ethiopia (see figure 1).
Disease Burden and the New Bottom Billion
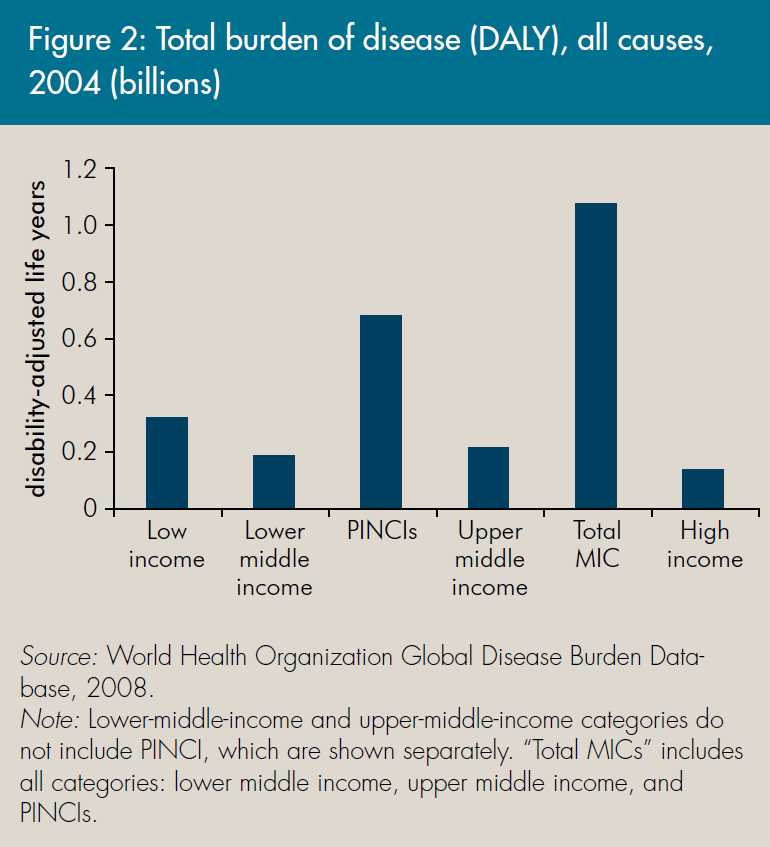
As countries that are home to the world's poor have graduated from LIC status, the distribution of the disease burden has shifted to the MICs. As a group, they now have a larger disease burden than LICs, in general and for specific diseases. The MIC disease burden is especially higher for vaccine-preventable diseases, but also for HIV/AIDS and tuberculosis. This disease burden is concentrated among the PINCI but is still significant in the non-PINCI lower-middle-income countries (LMICs) as well as-more surprisingly-the upper-middle-income countries (UMICs) in the case of HIV/AIDS.
The shift in disease burden to MICs is driven mainly by population size but also by lagging effort from the public health programs that prevent or control disease. The share of children who have received full childhood inoculations (the complete vaccination rate) is lower in many MICs than LICs. According to household survey data in 20 LICs and 17 LMICs, 42 percent of children under age five, on average, are fully vaccinated in LMICs versus 55 percent in LICs. Administrative data, generally considered to be of poorer quality than household survey data, provide a more encouraging picture but is still consistent with the patterns observed in household data. Beyond this, new vaccines that are often available in LICs, such as those against rotavirus, pneumococcal disease, and Hib, have yet to be introduced in many MICs. [3] Poor people in MICs also have greater difficulty accessing lifesaving HIV treatment than their LIC counterparts (see figure 3).
Global health agencies may have accentuated these patterns by favoring LICs in their funding allocations. In 2009, 46 percent of total health aid from Development Assistance Committee donors was directed to LICs, whereas 39 percent was directed to LMICs and 14 percent was directed to UMICs. [4]
Further, current health aid correlates poorly to disease burden. Some global health agencies, such as the GAVI Alliance, have set eligibility thresholds based on national income, which progressively disqualifies LMICs regardless of disease burden. In 2000, 72 countries were eligible for GAVI assistance; now 56 countries are eligible. Under GAVI's current policy, only 42 countries-half of the currently eligible population-will qualify for GAVI support by 2020. [5]
Donors seeking to improve health equity have no choice but to work in MICs, where most of the world's at-risk populations live. Health aid funding, like other aid, should respond to need, defined in this case as disease burden or size of at-risk populations, adjusted for the fiscal capacity of the recipient. Global health funders want to assure that cost-effective health technologies reach the poor, but, as we have seen, the LIC category is no longer a good proxy for the poor, nor is average income a good measure on which to base decisions about affordability or differential pricing structures since there is an extremely high concentration of wealth in MICs. [6]
Recommendations
It is important to distinguish between the different kinds of support for LICs and MICs. For LICs, direct resource transfers are necessary given their very low health spending per capita. For MICs, however, international support and partnerships can take different forms, many of which are not directly about resource flows. But there is still a role for a modest amount of global funding and facilitation that could leverage greater financing and better results in the MICs.
- Eliminate country-income thresholds or classifications as across-the-board eligibility criteria for global health funding
Global health agencies should recognize that effective aid allocation relies on more than a country's income classification. Using allocation methods that combine epidemiology, demography, and economics is ideal. The Global Fund has developed a prioritization model that looks at income, disease burden, and Technical Review Panel results. Similarly, allocation decisions could be made according to an index that combines disease burden and income level, which would benefit LMICs with worse health outcomes. Donors should not only base their activities on income thresholds but also incorporate the real objective of health aid, which is to improve health outcomes.
Similarly, global health agencies must develop a “big 5” strategy that reflects the specific barriers to change in the populous MICs. Many states or provinces within the most populous MICs would be classified as LICs if they were independent (for example, certain Indian states and Chinese regions).
- Set up regional pooled procurement schemes or negotiate an LMIC public-sector price within existing procurement mechanisms.
New vaccines are unaffordable in GAVI-eligible LMICs. Even under optimistic assumptions about growth and the priority given to health, national budgets in these countries will not be able to absorb the costs of new vaccines without GAVI support. GAVI's market-making ability has increased the volume of vaccines procured and provided greater certainty in available finance, which may have helped drive prices down. Widening the procurement pool-the market-would therefore benefit both LICs and MICs. To that end, global health agencies should encourage the pharmaceutical industry to deepen differentiated pricing strategies within MICs.
- Build evidence-based priority-setting institutions in middle-income countries
Neither GAVI nor the Global Fund requires countries to assess the budgetary impact of technologies before funding them, despite its critical importance to the sustainability of the disease prevention and control programs that the organizations support. While basic vaccines may be relatively uncontroversial and affordable, new vaccines demand more rigorous assessment. Such assessments could feed into evidence-based pricing and reimbursement decisions and would help countries use value-based pricing instead of external reference pricing in public or social insurance systems. An example of the potential for priority-setting institutions comes from Thailand's Health Intervention and Technology Assessment Program (HITAP) that decided against adopting the costly HPV vaccine in favor of a less expensive screening and treatment approach, which subsequently resulted in a more favorable price for the HPV vaccine.
- Establish increased accountability mechanisms and providing technical support to MICs
The global health community has done much to define the characteristics of “good” vaccination and infectious disease control programs. Yet country performance on financial and programmatic results is piecemeal, depends on self-reported administrative data, and has limited public visibility. Global health funders can do more to create reputational incentives for better performance on key public health priorities. In short, funders should nudge MIC governments into investing in the health of their populations by implementing results-based financing mechanisms and fostering global accountability through rankings that “name and shame” MICs with low public health spending.
Going Forward
Global health funders are at somewhat of a crossroads. In one direction, they could maintain the current model, phasing out some countries and allocating funds on the basis of average income per capita. This appeals to financially strapped donors, but fails to meet the global public health objectives that were the rationale for their creation. The other direction is for global health donors to engagement effectively with MICs, using some of the targeted strategies suggested here.
More detail on these recommendations, as well as the data underlying our policy analysis, can be found in the following working paper: Amanda Glassman, Denizhan Duran, and Andy Sumner, “Global Health and the New Bottom Billion: What Do Shifts in Global Poverty and the Global Disease Burden Mean for GAVI and the Global Fund?” CGD Working Paper 270 (Washington: Center for Global Development, 2011).
[1] Todd Moss and Ben Leo, “IDA at 65: Heading Toward Retirement or a Fragile Lease on Life?” CGD Working Paper 246 (Washington: Center for Global Development, 2011).
[2] Andy Sumner. “The New Bottom Billion: What If Most of the World's Poor Live in Middle-Income Countries?” CGD Brief (Washington: Center for Global Development, 2011).
[3] WHO, Global Burden of Disease Database (Geneva, 2008).
[4] OECD, CRS Database (Paris, 2009).
[5] GAVI's population drops from 328.6m in 2010 to 155.9m in 2020 (UN Population Forecasts; authors' analysis). We base our per capita income analysis on the IMF World Economic Outlook report until 2015, and extrapolate until 2020 by using the average predicted economic growth rate from 2010 to 2015.
[6] Prashant Yadav, “Differential Pricing for Pharmaceuticals” (London: DfID, 2010), http://www.dfid.gov.uk/Documents/ publications1/prd/diff-pcing-pharma.pdf, accessed August 2011.


