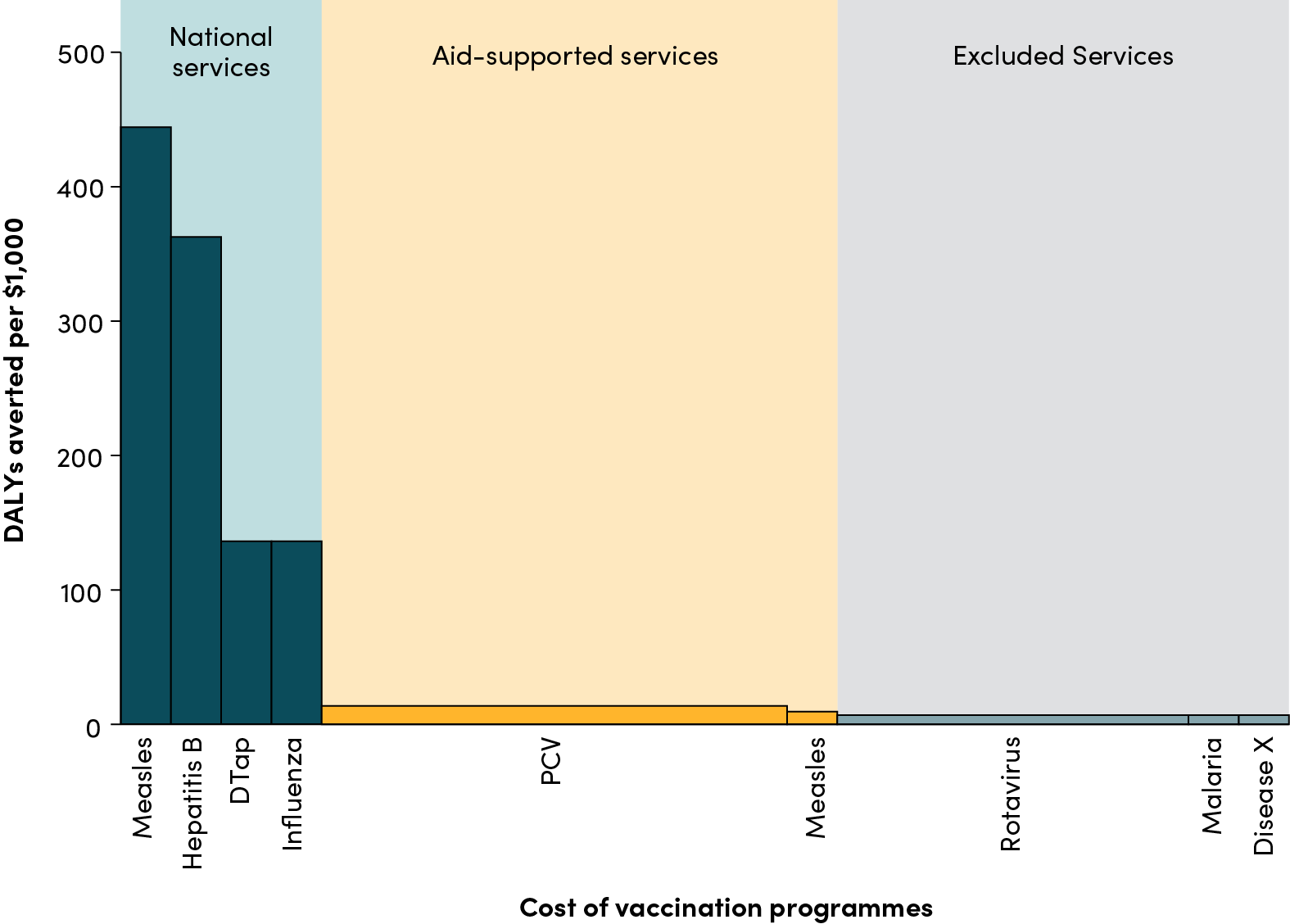
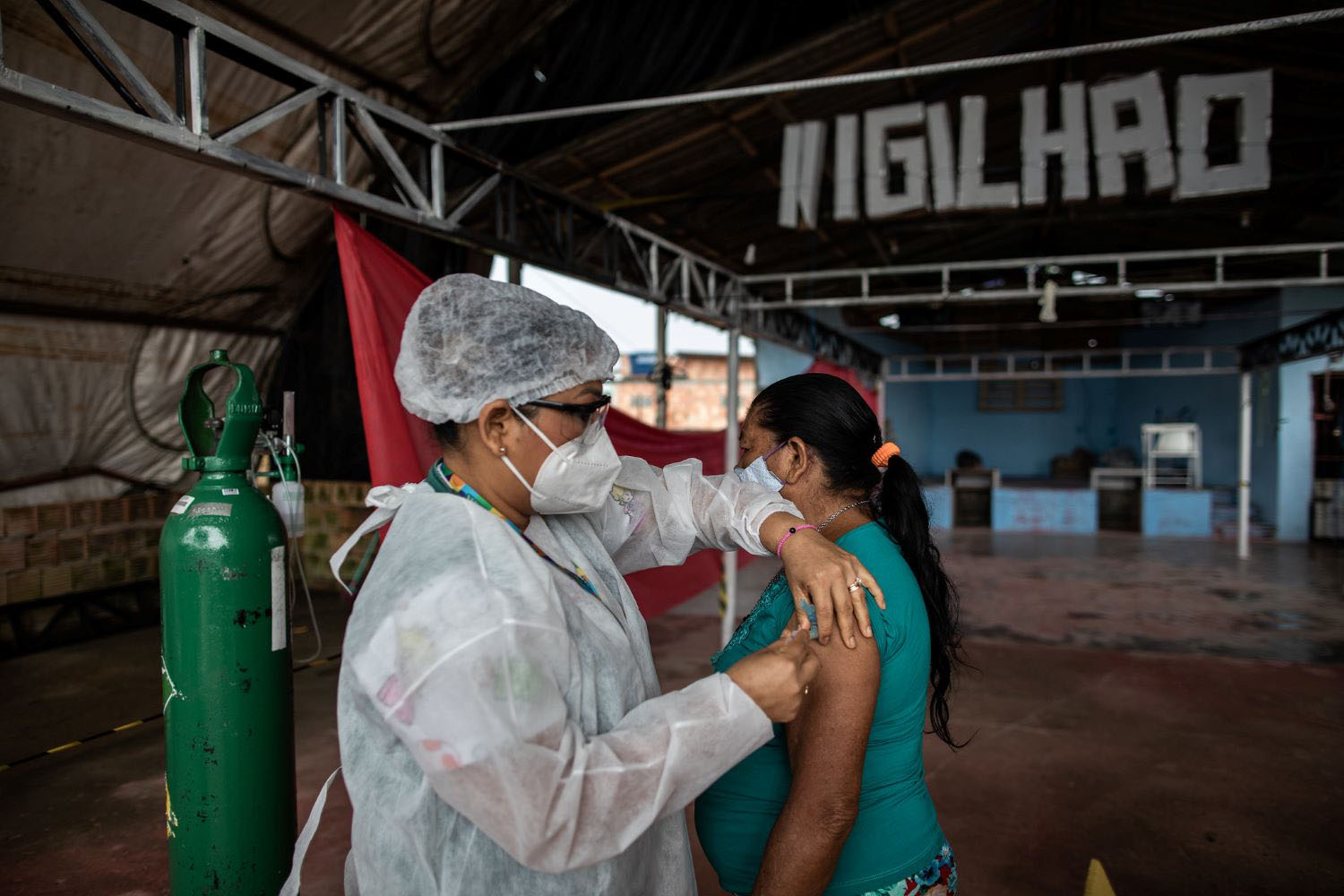
This week, Dr. Seth Berkley was named Chief Executive Officer of the GAVI Alliance. Expectations are high as GAVI seeks to raise US$ 3.7 billion this year for childhood vaccination in poor countries. Here are some ideas and questions for Dr. Berkley’s first day at work – welcome!1. Obtain fair share U.S. funding. Especially now that a U.S. citizen is CEO of GAVI, the U.S. should pony up some serious cash. No more free-riding on the Norwegians. I’ve written about this before here.2. Design and implement a long-term funding model. GAVI is no longer a temporary organization that can be funded by ad hoc replenishments. Full vaccination is a global public good that the poorest countries are unable to entirely finance in the short- and perhaps medium-term. Will GAVI lead on vaccination as a global public good? Can GAVI obtain some of the long-term, stable flows promised to global public goods as part of the G-20 and G-8 processes?The GAVI Board has recently re-emphasized its role as “market shaper” in order to drive down vaccine prices; however, this may be inconsistent with the goal of reducing the size of its procurements through country graduation. Given the cost structure of vaccine supply and the relatively small market and limited storability of most vaccines, competitive markets likely lead to one or very few suppliers in the long-run. When there is one supplier, a monopolist can set prices and the only alternative is negotiated tier pricing for poor countries based on longer-term commitments and/or larger volumes. Alternatively, we could see governments producing their own vaccines; Brazil’s Fiocruz Vaccine Manufacturing Center –which has partnered with GlaxoSmithKline in the past–is both a good bargaining tool and a potential model for the future.It would also be nice to harmonize GAVI and the Pan American Health Organization’s (PAHO) revolving fund purchasing strategies. It is not clear to an outsider how much the PAHO revolving fund’s lowest possible price clause will affect GAVI prices for new vaccines in the future, but both models have something teach each other in terms of sustainable approaches to vaccination financing. Here I am thinking about GAVI’s tiered price negotiations and PAHO’s procurement volumes and invoicing system that allows governments to pay bills later in a fiscal year when cash is more available.Can these different procurement models be combined? Could lower-income countries receive subsidized tier-priced vaccines while middle-income countries receive the benefits from pooled procurement prices? Could greater incentives for recipient country co-financing be built in? Are these goals inconsistent?3. Acknowledge and fund a double mission. In the past, GAVI has had to make allocation choices between investing in full coverage of existing vaccines and introducing new vaccines. If co-financing does not reach 100% on existing immunization in Africa in the next decade, what is the plan? Can a new Advance Market Commitment for malaria speed the introduction of this vaccine and mobilize additional resources? Perhaps it is time to acknowledge the mission as two-fold.4. Create a middle-income country strategy. Coverage inequalities in middle-income countries are also problematic and affect large numbers of poor children. GAVI’s decision to eliminate the middle-income countries is practical from a donor standpoint, but problematic from a public health perspective. How can incentives be created for full vaccination of the poor in middle-income countries? Should GAVI play a role? How does this choice affect the long-term funding model chosen?5. Consider the demand-side. GAVI’s model has focused on reducing the price of vaccines as the instrument to increase coverage. As the easy-to-reach are covered and coverage inequalities within countries increase, funding and programmatic attention should also be directed to the “demand-side” – impoverished mothers that face enormous financial, logistical, and knowledge barriers to obtain timely vaccination for their children. Impact evaluations from conditional cash transfer programs (see here) have shown significant effects on vaccination rates even in the context of adequate supply, suggesting that this dimension is important for timely vaccination of the poor. Does GAVI have the tools to support demand-side incentives?6. Consider using household surveys to measure vaccination coverage and reward performance. A major shortcoming of the otherwise-promising Immunization Strengthening Support (ISS) program was the variable quality of the immunization coverage estimates used to reward performance. Could GAVI and WHO evaluate the use of household surveys to measure and reward performance?I invite our reading audience to add their ideas and questions for GAVI’s new leader – what are your suggestions?
Disclaimer
CGD blog posts reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions.