Since 2019, the UK’s strong reputation in global health has been undermined by a series of cuts and a distracting departmental reorganisation. November 2023 may represent a turning point—with a new Foreign Minister who has historically championed aid as Prime Minister, and the publication of a new international development white paper. Depending on the results of an election, most likely in 2024, the future of UK global health will either be shaped by implementing this white paper, or by fresh ideas from a new government.
In this blog we highlight the key findings and recommendations from our new policy paper published today, which summarises the challenges and opportunities in global health that the UK has to navigate. We review UK global health aid expenditure data up to 2022, current UK global health policies, and the major external trends of the polycrisis era. Finally we conclude with a five-point plan that the UK should undertake in 2024 to focus its limited resources and restore its reputation.
UK global health cuts from 2018 to 2022—deep and off strategy
In 2018, the UK reported spending £2.17 billion (0.1 percent of Gross National Income (GNI)) on global health, which then rose as part of the COVID-19 response. But by 2022, it had fallen to £1.73 billion (0.07 percent of GNI) (see figure 1). If the UK had continued at its 2019 level of 0.1 percent of GNI, it would now have an additional £844 million to spend on global health annually—nearly an extra 50 percent. Bilateral programmes, FCDO-managed aid programmes, and reproductive health programmes were particularly hard hit by the cuts, despite the often-declared UK commitment to sexual and reproductive health and rights, and the Conservative 2019 manifesto’s commitment to “end the preventable deaths of mothers, new-born babies and children by 2030.” Going forward, future trends in UK global health expenditure remain uncertain, but there may be an increase in 2023 and 2024 due to reductions in expenditure on refugees in the UK and allocations to the EU. Increasing budgets offer an opportunity to deliver on the white paper objectives and restrengthen the connection between strategy and expenditure.
Figure 1: UK reported total global health expenditure as a % of GNI (Source: Statistics on International Development: Final UK Aid Spend 2022)
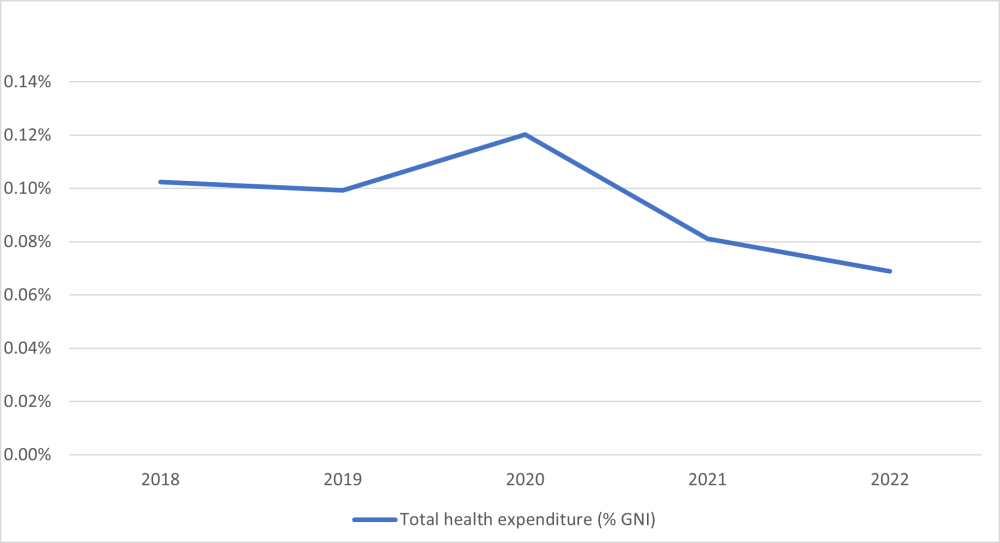
Note: 2022 multilateral data is not yet published and was estimated based on publicly available data—see Annex A in the policy paper
The UK must adjust its approach to the post-COVID polycrisis era
Implementing the white paper requires a clear consideration of current and future global health trends. Firstly, most low- and middle-income countries (LMICs) are facing a challenging health financing period. 110 LMICs are expected to have similar or lower government expenditure levels in 2027 than in 2019, representing an almost lost decade in raising the resources needed to make progress on universal health coverage (UHC) and the Sustainable Development Goals (SDG). Debt levels and interest rates are also rising, and 50 countries are spending over 10 percent of government revenues on debt repayments. The UK must similarly expect average domestic health financing to remain stagnant, possibly for the remainder of the SDG era, and that this will remain substantially below what is required to deliver a basic package of UHC services.
Secondly, demands on global health aid are changing. Population growth is concentrated in fewer, poorer countries, non-communicable diseases are on the rise, and global insecurity is increasing through zoonotic spillover events, antimicrobial resistance, and climate change. These global challenges require a coordinated, global response that strengthen the case for multilateralism.
Thirdly, following the pandemic there is a growing view that the current global architecture is not fit for purpose: pandemic preparedness lacked an effective mechanism for adequate global financing and coordination, global governance was slow to respond to COVID as it emerged, and the global COVID vaccine roll out was deeply inequitable.
A five-point plan for 2024
The white paper articulates core principles of the UK’s development agenda including eliminating poverty and focusing spend on the poorest countries, localised decision-making, long-term partnerships for strengthening health systems, multilateralism, the integration of climate and health agendas, and the centrality of sexual and reproductive rights. These tally well with the UK’s Global Health Framework and its Health System Strengthening (HSS) Position Paper. However, these papers lack clarity on priorities. The UK must come to terms with being a smaller player in global health, by improving the prioritisation (and de-prioritisation) of its global health financing. We therefore propose a five-point plan that would enable the UK to focus its resources and make progress on implementing the white paper:
-
Champion “more money for health” through debt relief and health taxes
-
Support countries to strengthen health system efficiency
-
Don’t try and do it all—track key priorities & focus on a few low-income countries
-
Conduct a multilateral aid review that empowers LMIC decision-making
-
Direct financing of health systems to the World Bank and bilateral programmes
Through these actions the UK can begin the long road to restore its reputation as a trusted development partner.







