When aid workers and expats pack for foreign postings their checklist is long. Yellow fever jab, malarial prophylaxis, insurance, and getting their kids enrolled in school. Lead poisoning rarely makes the list—but it probably should.
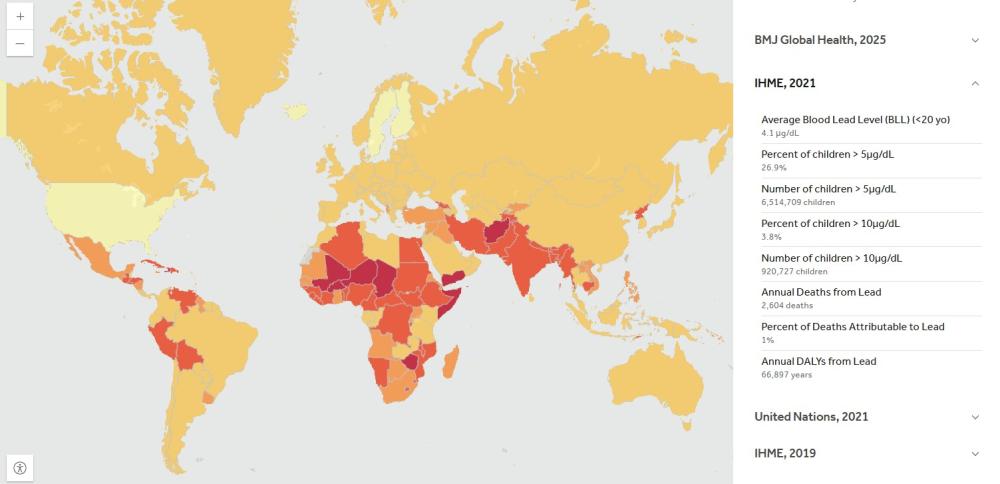
In half of low‑ and middle‑income countries (LMICs), the average child’s blood contains at least 5 µg/dL of lead. That is above the level that triggers public health action in Britain and the United States. Lead stunts brain development and raises blood pressure—and unlike malaria, it is hard to spot until the damage is done.
The best prevention of lead poisoning is also the most equitable—removing lead at the source, and protecting entire populations from its toxicity. That’s why we’ve called to end childhood lead poisoning for everyone by 2040—and why we’re so heartened to see recent funding and political commitments to that end.
But in the immediate term, international employers still have a duty of care for their staff. We argue that lead testing and mitigation should be included in this duty of care package for all expatriates in high burden-settings—including aid workers, diplomats, and deployed military families. In the US and UK, this should be considered a requirement to comply with workplace safety regulations—the Occupational Safety and Health Administration and the Health and Safety at Work Act, respectively—which require employers to take “reasonably practicable” steps to reduce workplace hazards. Plus, routine testing of expats will in turn help identify sources of local exposure that affect everyone—helping support host governments to find and clean up tainted consumer products and environmental pollution.
Note: Map reproduced from leadpollution.org, a project of Pure Earth
Wealth does not necessarily protect expatriates from lead
Isn’t lead poisoning a “poor people problem?” Not entirely. Anecdotally, one well-known American development economist told us that they’d discovered that their own children had elevated blood lead levels, after accompanying them on fieldwork trips in South America.
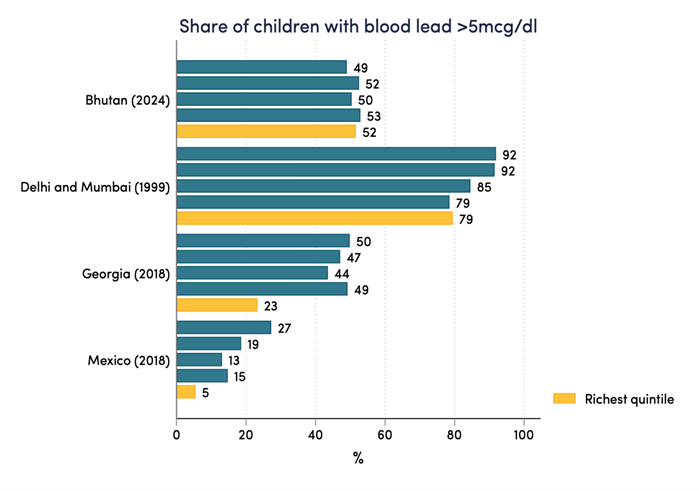
More broadly, we identified four large representative surveys that record both blood‑lead and household wealth; from India, Bhutan, Georgia, and Mexico. The richest fifth of households still show high numbers of children above 5 µg/dL. Gated compounds and international schools might help, but they cannot eliminate contaminated spices, water piped through lead‑soldered joints, or airborne dust from informal battery recycling a kilometre away.
Even children from richer families in poor countries have high blood lead levels
Note: This figure presents data on blood lead levels by wealth quintile from the 1999 National Family Health Survey in India, which included lead testing for Mumbai and New Delhi only; the 2024 National Blood Lead Survey in Bhutan; the 2018 MICS survey in Georgia; and the 2018 ENSANUT in Mexico.
What does this mean for HR departments?
What are reasonably practicable steps to address this problem? For malaria, for example, aid agencies subsidise bed nets, prophylaxis, and evacuation plans. Lead, in turn, demands three comparably cheap interventions:
- Test: a baseline venous blood‑lead test for staff and dependants before departure, repeated every six months in high‑prevalence posts. In Nairobi a lab test costs about $35—cheaper than most visa fees.
- Trace: if results exceed 5 µg/dL, investigate the source. Paint swabs and water test kits cost a few dollars;
- Treat—mostly the environment, not the person: chelation is rarely needed below 40 µg/dL. The priority is removing leaded items—repainting flaking walls, replacing pottery, or switching spices, for example.
The cost of testing and basic remediation comes to a small fraction of a typical embassy or country programme’s budget. In return, agencies avert lifelong health and cognitive penalties for their staff and their children.
Testing expats = more data for everyone
Routine testing of expatriates can also create a more equitable side benefit for the host country: evidence. New York City’s health department has identified imported lead-contaminated products such as spices and cookware, allowing the city to both protect New Yorkers and also to alert national authorities in Georgia. Aid agencies could do the same, amplifying their development impact at negligible cost. When expatriate families identify contaminated products, they can hand the proof to local regulators, adding pressure to clean up markets.
Don’t be the last to act
HR managers set travel rules and insurance requirements. Add blood‑lead testing to the checklist now and you safeguard your own staff–and, by flagging tainted products, you push local markets to clean up, protecting neighbouring families too. A minor line item in the budget can make a major dent in a toxin as old as plumbing.