Update: Here’s a recap of key moments from Friday’s #HealthForAll Twitter chat!
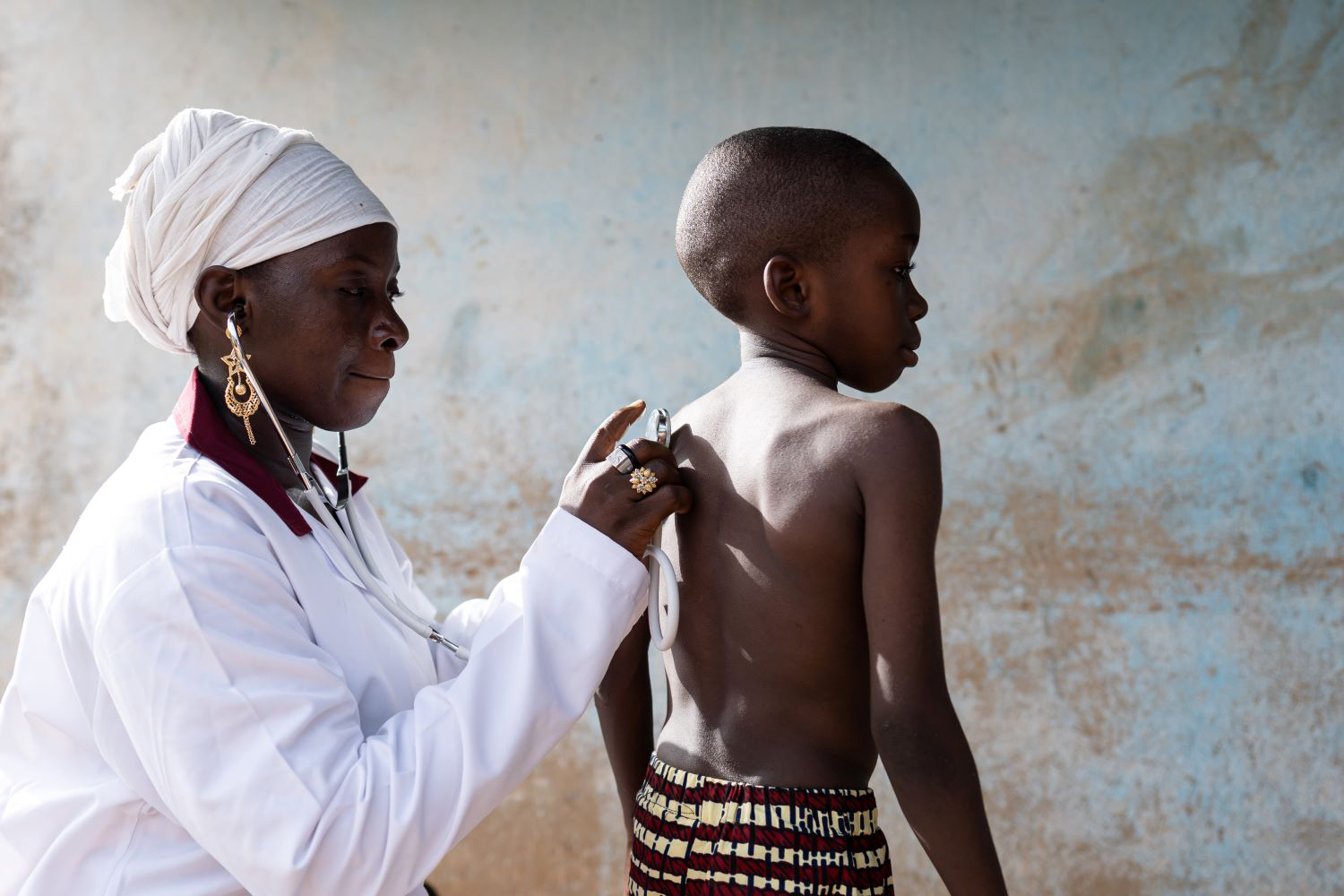
Each year, millions of people fall into poverty because they have to pay out of pocket for medical care. At least half of the world’s population does not have access to essential health services. Universal health coverage (UHC) is the goal of ensuring that everyone, everywhere can access quality health services without the risk of financial hardship.
We can make UHC happen in our lifetime by targeting investments and incentives on the highest impact interventions among the most affected populations in developing countries.
Starting Saturday, with World Health Day 2018, a drumbeat of activities will focus on increasing political will to advance health for all. The series of events include: the 71st World Health Assembly (WHA) in May, the United Nations General Assembly in September, and the marking of the 40th anniversary of the Alma-Ata Declaration in October in Almaty, Kazakhstan. It is anticipated that a new Alma-Ata Declaration will be set in motion and adopted at the WHA in 2019. These moments provide an opportunity to help shape and accelerate the UHC agenda.
Countries at all income levels are proving that UHC can be both achievable and affordable. However, current global funding has leveled off while the need for life-saving services and products has not. Governments and global health funders need to do more with existing resources.
Over the coming months, we at CGD will be highlighting three areas in particular that will impact efficiency and achieve more health for the same amount of money, particularly in low- and middle-income countries:
-
Adoption of an explicit, evidence-based Health Benefits Package—a defined list of services that are and are not subsidized—is essential in creating a sustainable UHC system. It is key to evaluate how much health an intervention will buy for each dollar.
-
Better data and performance verification—combined with results-based funding—is a powerful instrument for UHC mechanisms. There is the potential to improve efficiency of the health system and increase productivity of health workers, while ensuring quality, equitable services at an affordable cost.
-
More systematic use of health technology assessment of the comparative effectiveness and costs of health technologies will provide the economic and clinical evidence needed for decisions about what products to purchase to achieve greater impact for money spent.
Tomorrow, CGD (@CGDev) and I (@glassmanamanda) are looking forward to teaming up with Loyce Pace (@globalgamechngr) and the Global Health Council (@GlobalHealthOrg) for a Twitter Chat from 10-11am ET. By working together, we can share best practices towards greater efficiencies and improve access to quality health care services for everyone, everywhere.
Please join us on Friday using #HealthForAll.