Recommended

Event
Achieving UHC Requires Disinvestment as Well as Investment: Experience of Malaysia, Iran and Uganda
The Seventh Annual Health Financing Forum: Investing in Health in the post-COVID Era kicks off today in Washington DC, hosted by the World Bank, USAID, and the Global Financing Facility. It marks the 30th anniversary of the influential World Development Report 1993, Investing in Health. The organisers are seeking to promote greater government investment in health—an important mission but one that faces adverse fiscal and economic headwinds. Following the COVID-19 pandemic, health finances around the world are under pressure from weak economic growth and high debt repayments, and some are even cutting healthcare budgets. Even countries with growing economies and health budgets are still under pressure due to increasing demands from ageing populations, rising non-communicable diseases, and universal health coverage (UHC) aspirations.
One solution that is often proposed to square this circle is one of the most politically difficult issues in health financing: disinvesting in low priority and low-impact healthcare services. This releases money for high priority services and can, in theory, enable countries to make progress on UHC ambitions, even when budgets are tight. In this blog, and in a CGD policy paper released today, we summarise examples of healthcare disinvestment in low- and middle-income countries (LMICs) to draw insights on what has and has not worked.
We found four documented examples of one-off disinvestment initiatives, two documented examples of systematic disinvestment initiatives by health technology assessment (HTA) agencies in LMICs, as well as a range of countries like Thailand, India, and Ghana that carry out systematic disinvestment through routine HTA processes. We conclude that disinvestment is costly, time-consuming, and rarely as successful as policymakers intend. Key considerations to improve the chances of success include whether strong pre-existing health prioritisation systems exist (such as an HTA agency) and whether the design of initiatives are tightly matched to the level of political will, the policy objective, and available resources.
Why does disinvestment so often fail?
Fundamentally, the challenge is that healthcare disinvestment is difficult and costly— technically, organisationally, and politically. Because disinvestment involves removing or restricting access to a health technology, it can provoke resistance from the public, politicians, and health professionals. Even when disinvestment is tied to re-investment, for example through replacement of an old technology with a new technology, or through savings being reallocated elsewhere in the health system, it still produces winners and losers, which results in political tension and resistance. The result of this resistance is that when initiatives reach implementation, what gets done is usually a fraction of what was initially proposed and, consequently, benefits tend to be much less impressive than expected. Moreover, the promise of reallocating freed resources is contingent on having sufficient flexibility to reallocate health budgets. These conditions are not easy to meet, particularly in low-resource settings.
Two types of disinvestment initiatives—one-off and systematic
We found that disinvestment initiatives in LMICs can be described in two stereotyped scenarios. Firstly there are “one-off” initiatives, typically focused on a single objective such as cost cutting; such initiatives are conducted usually with highly constrained resources and priority-setting expertise, and with high initial political will that has a tendency to fade when the project inevitably takes longer than expected. Examples of this in the paper include Vietnam, Romania, Iran, and Malaysia. Rapid reviews with a defined and limited scope may have resulted in less resistance and easier implementation, but it was notable that the impact in all these examples was much less than intended or recommended initially.
Secondly there are larger scale “systematic” initiatives, often led by established HTA agencies with substantial resources and time. They are backed by sustained political will, and a broad set of objectives to improve value for money in the health system. Some HTA institutions, such as in Brazil and China, established a specific disinvestment workstream to do this, others such as Thailand, India, and Ghana used their routine HTA processes to gradually review and disinvest from technologies and replace them with newer or preferred alternatives. All of these approaches have had success, suggesting that long-term investment in effective priority-setting institutions has the valuable side effect of enabling more successful disinvestment initiatives.
What can increase the chance of success?
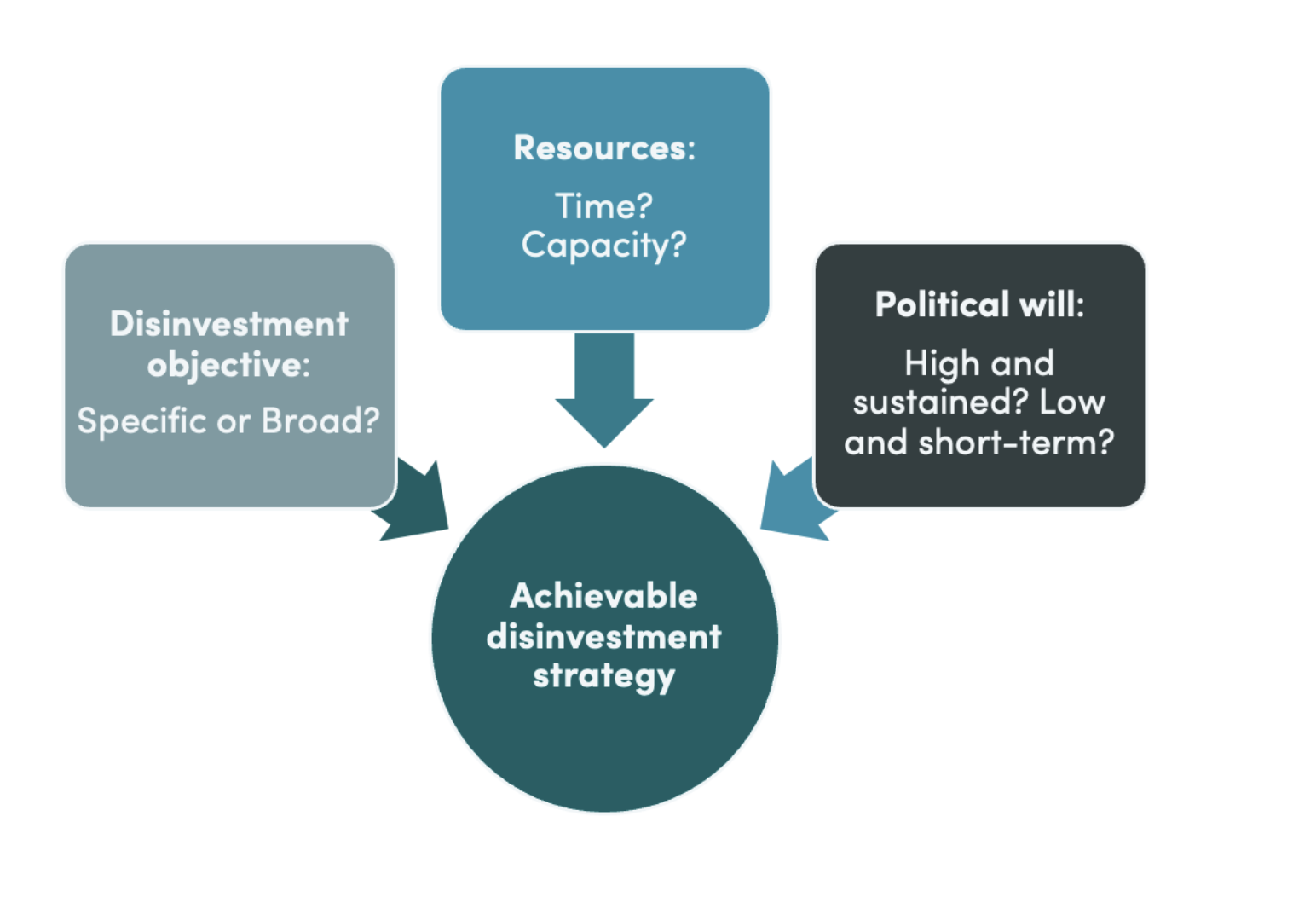
Success of a given healthcare disinvestment strategy appeared to be influenced by matching the approach to three key contextual factors (figure 1):
1. The disinvestment objective: is the disinvestment initiative focusing on a single, policy objective (e.g., cost cutting) or does it have multiple, explicit policy objectives, in which case a more elaborate design is often needed?
2. The political will: does the ambition of the project match the extent of the mandate and likely duration of support from senior leadership?
3. The resources available: how much time is available before a decision needs to be made? Are there sufficient skilled people, relevant data, financial resources available?
Figure 1. Three factors to consider when designing an achievable disinvestment strategy
Conclusion
In theory, disinvestment offers the potential to release resources for achieving UHC during challenging fiscal times. However, in practice, it is time- and resource-consuming and results in less benefit than expected at the outset. The opportunity cost of launching an initiative needs to be weighed against other health policy reforms, particularly in low-resource settings. Before beginning a disinvestment programme, we offer four recommendations for decision-makers, based on the limited evidence available:
- Consider which of the two scenarios you are in and make sure expectations and approach are well matched to three contextual factors—disinvestment purpose, political will, and available resources. Aim too high or too low and you will waste resources, damage credibility, and breed disappointment; aim at the right level, and you can achieve tangible gains.
- Be strategic about restricting the scope to where disinvestment can lead to improvements. Pilot initiatives restricted to vertical disease programmes or specific types of health technologies, at least as a stepping stone towards further developments. This can be promising and face less resistance, but it should be accepted that these initiatives may not produce large impact in the short-term.
- Evaluate and publish all disinvestment initiatives to support future policymakers on this critical area.
- Over the long-term, invest in priority-setting institutions (such as HTA) as the foundation for making difficult trade-offs routinely and systematically.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.