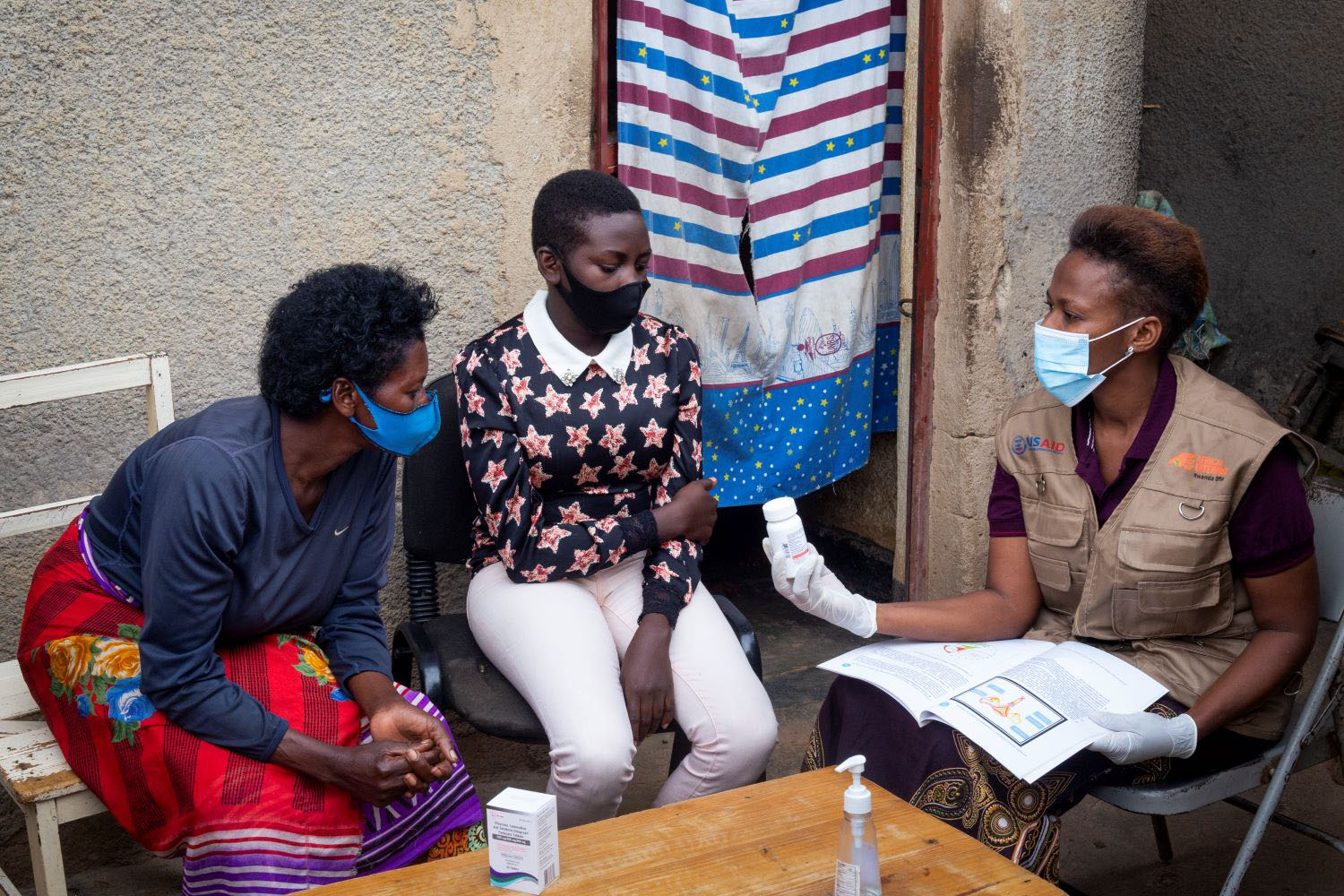
Back in February, the US Council of Economic Advisers issued a white paper on drug pricing implying that other rich countries should stop “free riding” off American innovation by negotiating drug prices to unfairly low levels after the US fronts the research and development costs. Perhaps in response, President Trump recently announced a proposal to bring down US drug prices. But until the US corrects the structural flaws in its own healthcare system, these efforts are bound to fall short.
President Trump’s plan faces an uphill battle
President Trump’s plan centers on an “international price index” model. The proposal focuses on one part of Medicare (the government program for people over 65): Part B, which covers drugs administered to patients by physicians, compared to Part D, which is nearly five times larger and covers drugs dispensed by pharmacies.
Projected to save $17.2 billion over five years, the proposal would introduce an experimental plan to be tested in half the country, with three approaches aimed at reducing the price of on-patent drugs:
-
Externally referencing prices to 16 other high-income countries
-
Introducing private vendors to aggregate volumes for negotiated discounts
-
Separating the cost of drugs from physician compensation
The proposal is likely to face significant challenges, including pushback from pharmaceutical companies against “price controls,” from physicians concerned about making less money, and from lawmakers and pharma lobbyists. It is also possible that pharmaceutical companies will refuse to offer the lower prices that the index projects, leaving patients vulnerable to lack of access.
The president’s plan has the potential to reduce prices, but given that Medicare Part B represents only a small proportion of the $457 billion annual total prescription drug spend in the US, it may not be enough to curb the country’s escalating drugs bill. What’s more, the issue of rising drug prices in the US is far more complicated than the Europeans and Canadians free riding off the US. Here’s why:
The size of the US pharmaceutical market is distorting pricing worldwide
It is true that on-patent drug prices are significantly higher in the US than in other high-income countries, but it is that very fact that distorts markets outside the US, not the other way around.
A quick macro-lesson on how the US market functions compared to its peers: most high-income countries have tax-funded or social-insurance-based health systems that aim to get the biggest bang for their public monies’ buck. With a set budget, many of these countries (e.g., the UK, Australia, Norway, Canada, New Zealand) set an implicit or explicit “willingness to pay” for a given unit of health (e.g., quality adjusted life year), which is grounded in each country’s budget, political priorities, and social values, and which helps payers decide whether to pay for a new treatment. Even those countries with less explicit, analytically, approaches—such as Germany, Japan, and France—tend to negotiate prices based on proven clinical value added.
In contrast, the US market is fragmented across the public and private sectors. Its loosely regulated public budgets rise through congressional appropriations to accommodate spending increases and are largely administered through a byzantine network of private plans, while private insurers increase their premiums year after year to sustain their margins, adding to the ranks of underinsured and uninsured. In both instances, the drugs’ bill is uncontrolled. (Check out the enormous share of the Medicare bill in the US budget here.) Unlike its European and Canadian counterparts, Medicare is not allowed to negotiate prices (though this may change soon), and public and private payers alike must abide by market-distorting regulations such as covering all cancer products with FDA approval at the manufacturer’s asking price. We’ll cover more (and equally distorting) qualities unique to the US market a bit later.
The flipside of the free-riding argument is one where the US market is a source of global inefficiency, setting the reimbursement bar inappropriately high for new technologies and hence putting pressure on EU and other markets (e.g., Japan, Canada, Australia, and even some lower-middle-income countries) to pay more than they ought to given incremental benefits conferred by the latest innovation and alternative demands on their finite budgets. US pricing and coverage decisions increasingly serve as a benchmark even in much poorer countries. Faced with increasing demand for innovative treatments, but lacking the bargaining power and capacity to evaluate the value of these new treatments in their own settings, lower-middle-income countries can succumb to pressure to introduce overly expensive treatments, like South Africa recently did with a new breast cancer treatment. In a system that has neither the capacity to screen, diagnose, and intervene early, nor to provide adequate palliative care for advanced cases, the treatment was approved at too high a price, with limited to no budgetary allocations at provincial levels (in South Africa, provinces pay for drugs out of their own budgets).
In addition to the inflationary impact of the US market on other countries, current pharmaceutical investments disproportionately focus on the much-more profitable disease burden of American patients. This leaves a significant gap in global R&D investments for neglected diseases—those more prevalent in poor countries that do not attract pharmaceutical investment (e.g., malaria, tuberculosis, and diarrheal diseases).
Other countries are adopting HTA and driving prices further down; the US should take note
As the US debates how to manage its escalating drug prices by externally referencing prices (a move that US Secretary of Health and Human Services Alex Azar admits could limit drug access elsewhere), countries worldwide are working to bring down the costs of innovative products while expanding access for their populations in need.
A growing number of countries are using health technology assessment (HTA) as a mechanism for considering evidence of comparative value (clinical and economic) of new products in order to identify appropriate price levels and serve as a starting point in price negotiations:
-
The European Commission recently proposed to reinforce cross-country collaboration on HTA, which would enable joint clinical assessments, scientific consultation, and identification of emerging technologies.
-
A subset of EU countries—Belgium, the Netherlands, Luxemburg, Austria and, more recently, Ireland—formed a pricing collaborative, “BeNeLuxA,” aimed at reducing the price of orphan drugs. It recently negotiated its first successful price deal, on Spinraza, based on value to the participating healthcare systems and on the overall budgetary envelopes.
-
In India, the government completed and published its first HTA on a medical technology setting out ceiling prices for intraocular lenses. These prices are likely to inform Modicare’s reimbursement schedule; this is the first of many analyses underway in the country’s new national HTA body.
-
In China, the price of 17 oncology drugs was decreased by 50 percent on average, building on advice by the National Center of Medicine and HTA, launched in Beijing in October 2018.
These are just a few examples—a table summarizing major HTA initiatives is below.
Regulatory and structural issues within the US allow pharmaceutical companies to influence politicians, patients, and physicians—directly and indirectly affecting prices and profits
President Trump’s proposed international price index would tackle only a small portion of pharmaceutical companies’ influence on pricing, policy, and prescribing. In addition to Medicare being unable to negotiate prices, the pharmaceutical industry can and does ramp up prices yearly (unlike other OECD markets, where such practices are disallowed) and “evergreens” drugs to extend patents (and thus monopoly power) far beyond 20 years. In the same vein, the pharmaceutical industry in the US spends $5 billion per year on direct-to-consumer advertising (again, illegal in most OECD countries), another $216 million annually lobbying Congress, and on average $61,000 per physician annually to influence prescribing practices.
Introducing externally referenced prices and pegging US prices to those of, say, the UK, Canada, or Australia, with the kind of “socialized” healthcare systems many in the US are averse to, is a sensationalist move. Even if implemented for more than Part B and across the whole country, President Trump’s proposal is unlikely to yield lasting savings as long as major structural paradoxes in the US system remain. What it will do, however, is satisfy the administration’s rhetoric about other countries free riding on US generosity and good will.
Drug prices in the US are too high. Rather than lay the blame on other countries’ healthcare systems, the US should start mending its own system, removing perverse incentives and tackling its (made in America) rent-seeking practices.
Worldwide Summary of Major HTA Initiatives
| Emerging Markets | ||
|---|---|---|
|
China 
|
“We have fully utilized HTA…to balance financially sustainability and access to new cancer drugs…up to 30% price reductions compared to nearby countries.” Director of Chinese Medical Insurance Bureau, Beijing, October 2018 |
|
|
India 
|
“The India Medical Technology Assessment Board for evaluation and appropriateness and cost effectiveness of the available and new Health Technologies in India…standardized cost-effective interventions that will reduce the cost and variations in care, expenditure on medical equipment…overall cost of treatment, reduction in out of pocket expenditure of patients.” MTAB, Ministry of Health & Family Welfare, Government of India |
|
|
Indonesia 
|
(5) Health Technology Assessment Committee provide policy recommendation to the Minister on the feasibility of the health service as referred to in paragraph (4) to be included as benefit package of National Health Insurance Indonesia: Minister of Health’s Decree No. 71 /2013 Article 34 |
|
|
Philippines 
|
“The Corporation shall not cover expenses for health services which the Corporation and the DOH consider cost-ineffective through health technology assessment.” National Health Insurance Act of 2013, Section 11- Excluded Personal Health Services |
|
|
South Africa 
|
Service coverage (5.3): South Africa “Detailed treatment guidelines, based on available evidence about cost-effective interventions, will be used to guide the delivery of comprehensive health entitlements. Treatment guidelines will be based on evidence regarding the most cost-effective interventions.” RSA National Treasury (HTA unit budgeted @R368m in 2018 Treasury budget) |
|
| Low- and Middle-Income Markets | ||
|
Ghana 
|
“MOH should develop a transition plan to ensure sustainable financing and operational management of the supply chain to transition to a government led supply chain system; MOH should establish a National Pricing Committee for Medicines; MOH should institutionalise Health Technology Assessment to provide technical advice to the NPC.” Ghanaian National Medicines Policy |
|
|
Kenya

|
“Define an evidence-based benefit package for Kenyans under Universal Health Coverage: (A list of services that should be prioritized and made available taking into account the cost effectiveness, impact on financial protection, and equity in access across the population). - Define a framework for institutionalization of Health Technology Assessment (HTA).” Cabinet Secretary, Government Gazette, July 2018 |
|
|
Tanzania 
|
“The aim of the Tanzanian Health Technology Assessment Committee (THTAC) is to make evidence-informed recommendations to the MOHCDGEC based on the internationally recognized HTA framework. The committee will make recommendations about the public provision of health technologies that will contribute to maintaining and improving the health and well-being of Tanzanians, provide value for money and lead to the ultimate goal of Universal Health Care.” TANZANIA HEALTH TECHNOLOGY ASSESSMENT COMMITTEE (THTAC) Report, 2018 “The government will improve adequate knowledge in health technology assessment (HTA) for evidence-based selection of quality and safe technology as well as realizing value for money.” 2017 National Health Policy 5.14.3. Policy Statements |
|
| High-Income Markets | ||
|
European Union Commission 
|
“The outcome of HTA is used to inform decisions concerning the allocation of budgetary resources in the field of health, for example, in relation to establishing the pricing or reimbursement levels of health technologies. HTA can therefore assist Member States in creating and maintaining sustainable healthcare systems and to stimulate innovation that delivers better outcomes for patients.” REGULATION OF THE EUROPEAN PARLIAMENT AND OF THE COUNCIL on health technology assessment and amending Directive 2011/24/EU |
|
|
BeneLuxA + Ireland 
|
“The initiative aims to achieve its goals by … increasing efficiency in the assessment, pricing, and reimbursement of pharmaceutical products by exchanging expertise and the mutual recognition of HTA.” BeNeLuxA Initiative on Pharmaceutical Policy Terms of Reference |
|
Topics
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.