Over the last twenty years, many low-and middle-income countries (LMICs) have begun to develop health benefits packages (HBPs), which are lists of prioritised services or interventions funded with public monies as part of plans to achieve Universal Health Coverage (UHC).
HBPs are considered an essential element of a sustainable and effective health systems. They help governments explicitly define what services are critical to be publicly funded, and what services are desirable but not essential, given budget constraints, which is core to the UHC mandate. However, political and practical challenges have hampered priority setting efforts and the development and revision of HBPs in several LMICs.
One of the reasons why prioritisation is so challenging is that the cost of delivering the list of services needs to be balanced against the funding available for health systems in order to be sustainable. This is especially difficult in many LMICs, where public spending on health is still extremely low and other healthcare resources tend to be limited: in 2018, domestic current health expenditure was less than $10 per person in twenty two countries. The disconnect between aspirational health plans and available resources is the single most common failing of existing benefits plans.
HPBs are also not a static output: once they are developed, countries need to review regularly to ensure that the package of services, goods, and health commodities are still appropriate for the health needs of the population, incorporate the emergence of new evidence on existing services, and address the changing amounts of resources available to finance the HBP. Revisions may also be necessary to course correct following implementation and address issues that have been identified once the first version of the health benefit package is rolled out.
So, what are the main implementation challenges encountered by countries in developing and updating their health benefit packages? And how have they managed revisions in the past?
We worked with the Joint Learning Network (JLN) Efficiency Collaborative to gain insights from Collaborative members who represent technical staff and decision-makers working at the heart of health benefit packages development and revisions in eleven low-and middle-income countries in Africa and Asia (Bangladesh, Ethiopia, Ghana, Indonesia, Kenya, Laos, Malaysia, Mongolia, Nigeria, Philippines and Sudan). This blog summarizes the initial results from a survey conducted earlier this year to capture their views and experiences on the HPB development and updating process.
1. Almost all countries in the Efficiency Collaborative have a health benefit package, with experience spanning over twenty years
Almost all countries reported that they have developed a health benefit packages that is implemented in practice. In this context, implementation means having at least i) a funding pool to support its delivery, ii) funding lines to reimburse providers for the provision of services or iii) entitlements enshrined in law (definition from Regan et al.) We expanded the definition to add that the benefits package is also currently being delivered. The only exception is Ethiopia, whose health benefit package has been recently reviewed and for which implementation strategies are currently being drawn. The oldest health benefit packages identified in the group were in Sudan (1994) and the Philippines (1995).
2. Respondents identified clarity of entitlements, increase equity of access, facilitated planning and alignment with disease burden as the main benefits associated with HBPs in their settings
The respondents to the survey were asked to comment on any of the benefits of developing a health benefit package in their settings. One respondent stated that it makes it easier for decision-makers to understand what their funds are spent on, including for the Ministry of Finance. Another country mentioned the benefits in terms of guarantees for patients: equitable access, quality and affordability of services (including financial protection). Finally, several respondents emphasized the benefit of a health benefit package to ensure that funding was spent on most prevalent conditions and addressed the burden of disease adequately.
3. Too many high-cost interventions alongside insufficient financial resources appear to be the two leading problems when implementing health benefit packages
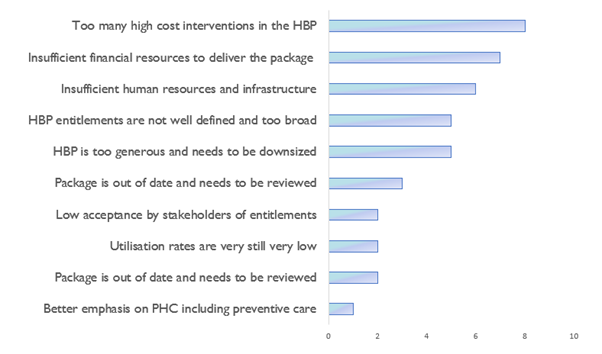
All countries with an implemented health benefit package reported challenges during the roll-out. The most cited problems were ‘too many high-cost interventions in the HBP’ and ‘insufficient financial resources to deliver the package’.
Figure 1. What are the biggest challenges of implementing existing HBPs?
N.B. In some cases, there was more than one respondent per country and we constrained the number of challenges to three
4. Revisions can take many forms and occur at different intervals
Most countries reported experience with revisions but we found that this could occur in many ways. Revisions can be different in each country, and the literature hasn’t developed a clear typology. According to our survey, a revision was understood as a change in entitlements (a removal or an addition), a whole review leading to changing a set of entitlements, a change in the way the entitlements were specified or a change in focus, delivery modality or tariffs (payment of provider).
The survey showed that removals to entitlements were less common, and almost half of the respondents noted that their revisions consisted in adding a set of services or interventions to the package.
A revision can be triggered by changing circumstances. Most recently, several countries have expressed concerns, for instance, about declining fiscal resources (including in the healthcare sector) as a result of the COVID-19 pandemic. However, changes in fiscal space, disease burden and available treatments or even broader health system reform were all identified as potential reasons for revisions. This may prompt the need to reshape the health benefit package to meet those anticipated changes in both health needs and fiscal space. Some countries put in place provisions to revise the health benefit package periodically. From the literature, we found that Colombia and Chile revise their plan every two years and from the survey we found that the Philippines’ PhilHealth has periodic revisions, but these aren’t conducted on a specified timeframe. However, it is worth noting that few countries had legal provisions for periodic revisions, suggesting that revisions were generally initiated to address a specific challenge that emerged.
5. Long timelines, insufficient expertise, lack of political support and a lack of data and evidence made revisions difficult in the countries surveyed
Most respondents stated in the survey that challenges were identified during revisions, and many types of challenges were identified, including difficulties with generating and incorporating data and evidence, designing a transparent process, and political economy.
Long timelines for revisions were highlighted as problematic. One respondent stated:
“It takes longer than expected, managing large numbers of clinical expert groups is very challenging, but good advocacy and engagement of high-level policy makers was essential and with good impact.”
Another respondent from a different country explains:
“Initially step by step new diseases were included in the package after consultation with relevant experts and later finalized and approved by authority. It is already reviewed two times and from beginning of HBP revision to finalization, it took almost 4 years.”
On the other hand, a quick process also seems to be unproductive. One respondent noted that a ‘quick revision’ was done in a month in their country, but because of the lack of consultation and transparency, it was never used.
Conclusion
Developing a health benefit package that is responsive to health needs and is financially sustainable has been identified as one of the most important challenges on the journey to UHC.
Most countries have developed a health benefits package and found that, whilst they have many benefits, there are implementation challenges linked to their sustainability and suitability. Revisions are essential to ensure that health benefit packages deliver effectively, but there is a lack of guidance in the literature on how to improve the revisions process and increase the quality of decision-making.
A potential solution can be found in co-learning and sharing country experiences, both positive or negative, on how revisions were conducted and how they can be improved. Working towards this goal, the responses to this survey will feed into the next JLN knowledge product, to be released early next year. This resource will provide a roadmap on health benefit packages revision, which will be informed by case studies and lessons learned based on real-world country experiences.
This blog post builds on qualitative information provided by the respondents to our survey. There may be inaccuracies, biases and it is in no way intending to reflect the challenges and experiences of all low-and middle-income countries (or of the regions we cover). However, they provide fascinating insights from the countries on their experiences with health benefit package reforms which is crucial as this is such an under reported area in the literature. Many thanks to our respondents and members of the Efficiency Collaborative.
Topics
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.