The world desperately needs new antibiotics—and finally, the G7 is ready match commitments with action. The United Kingdom (UK) has already launched a subscription purchasing model for two antibiotics and is considering a scale-up, while new programs to incentivize antibiotic research and development (R&D) are under consideration in the United States (US), European Union (EU), Canada, and Japan.
A few weeks ago, we estimated the expected return on investment (ROI) to the US government for an ambitious new program to bring 18 antibiotics to market over the next three decades, targeted at the six priority pathogens that cause the most deaths. We found that the US would pay $17.9 billion over 30 years but save 383,000 American lives and harvest $495 billion in value—an ROI of 28:1. We assumed that the US would pay its “fair share” of the total global incentive cost, proportionate to its GDP within the G7 + EU—46 percent.
This, of course, begs the question: what would be the benefits to other members of the G7, who would be footing the rest of the bill? Today, we’ve done those calculations—and we can confidently project that all G7 members would see a big payoff.
Costs, benefits, and baseline resistance differ across the G7…
G7 countries are a heterogenous group across many different dimensions, including population, GDP, health expenditure, and baseline levels of antibiotic resistance. We do our best to account for those differences in our calculations, using local data whenever possible.
First, G7 members would contribute different amounts into the overall pot. We assume a total incentive of $4.5 billion is needed per drug. We split those costs among the G7 + EU members by a “fair share” methodology relative to each member’s 2021 GDP (Table 1).
Table 1. Fair share calculation
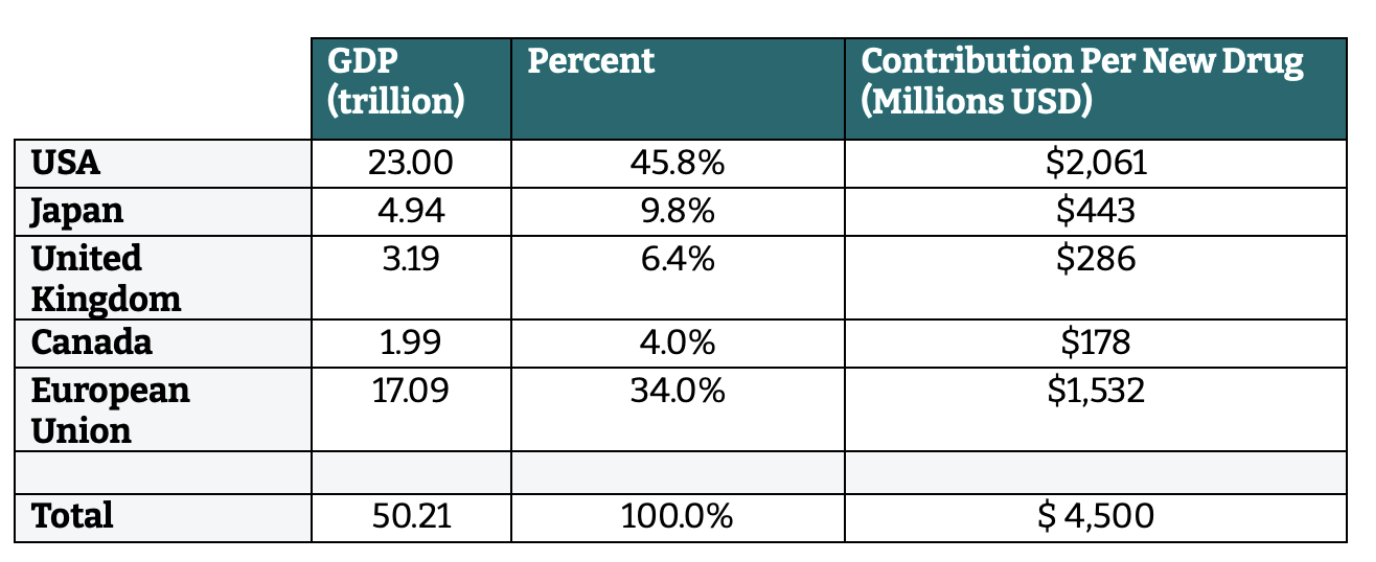
Source: World Bank Databank, using OECD
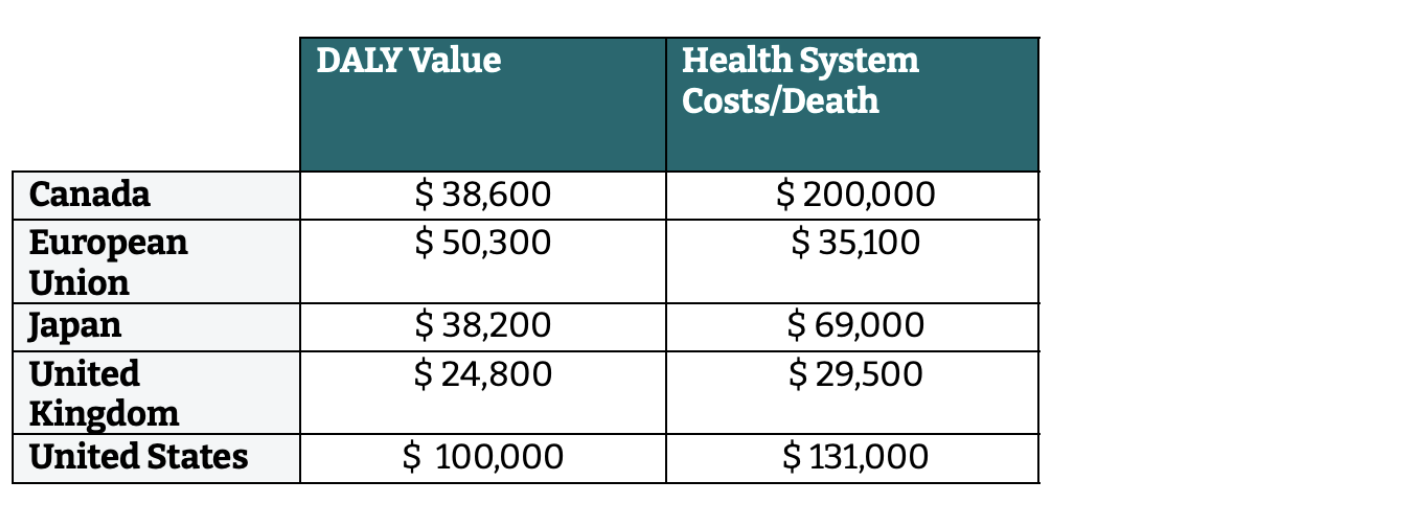
Second, G7 members vary substantially in their willingness to pay for a disability-adjusted life year (DALY) given current health expenditure, as well as the health system costs associated with antimicrobial resistance (AMR). We dig into each member’s cost-effectiveness thresholds and health expenditure to come up with our best-guess DALY values and health system costs associated with an AMR death. We use USD (at average 2022 exchange rates) for consistency and err on the conservative side where relevant, e.g. using the lower end of a threshold range.
Table 2. Cost per DALY and hospital costs per AMR death, by G7 member
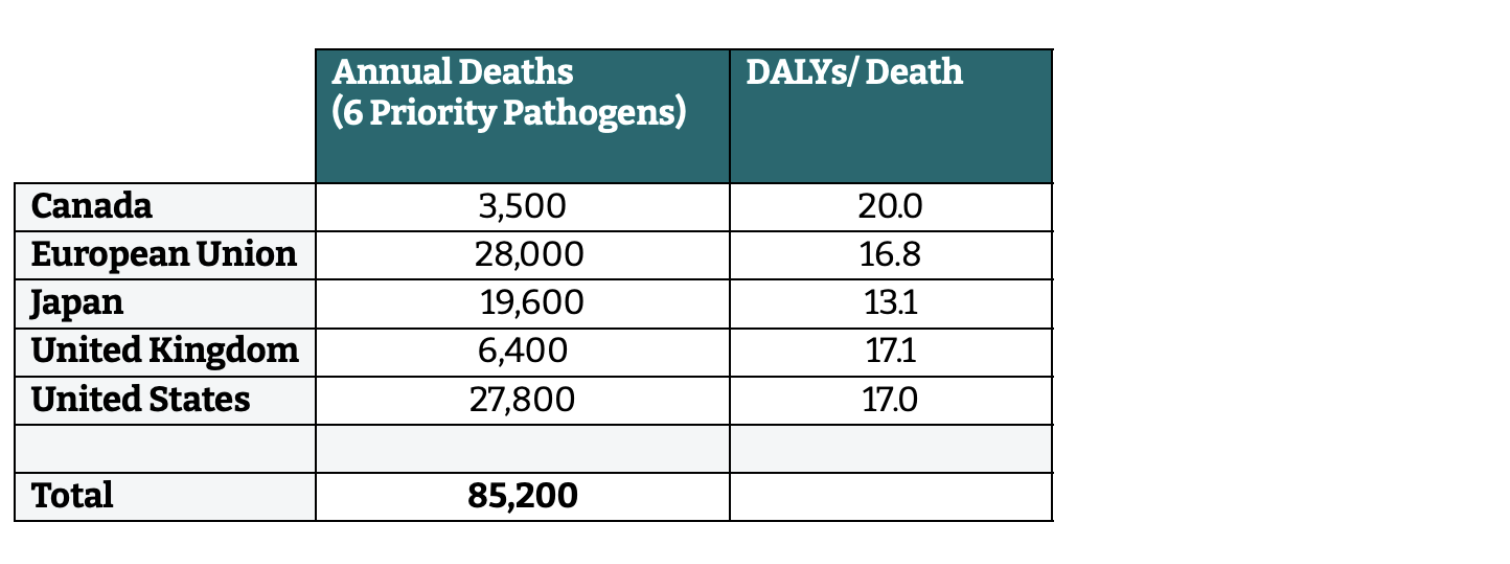
Finally, G7 members have different starting points for the level of AMR deaths. We use a mix of international estimates and local data to estimate the number of deaths attributable to six priority pathogens, as well as the average number of DALYs associated with each death (Table 3).
Table 3. Baseline deaths and DALYs per death attributable to six priority pathogens, by G7 member
…But new antibiotics are a good investment for everyone
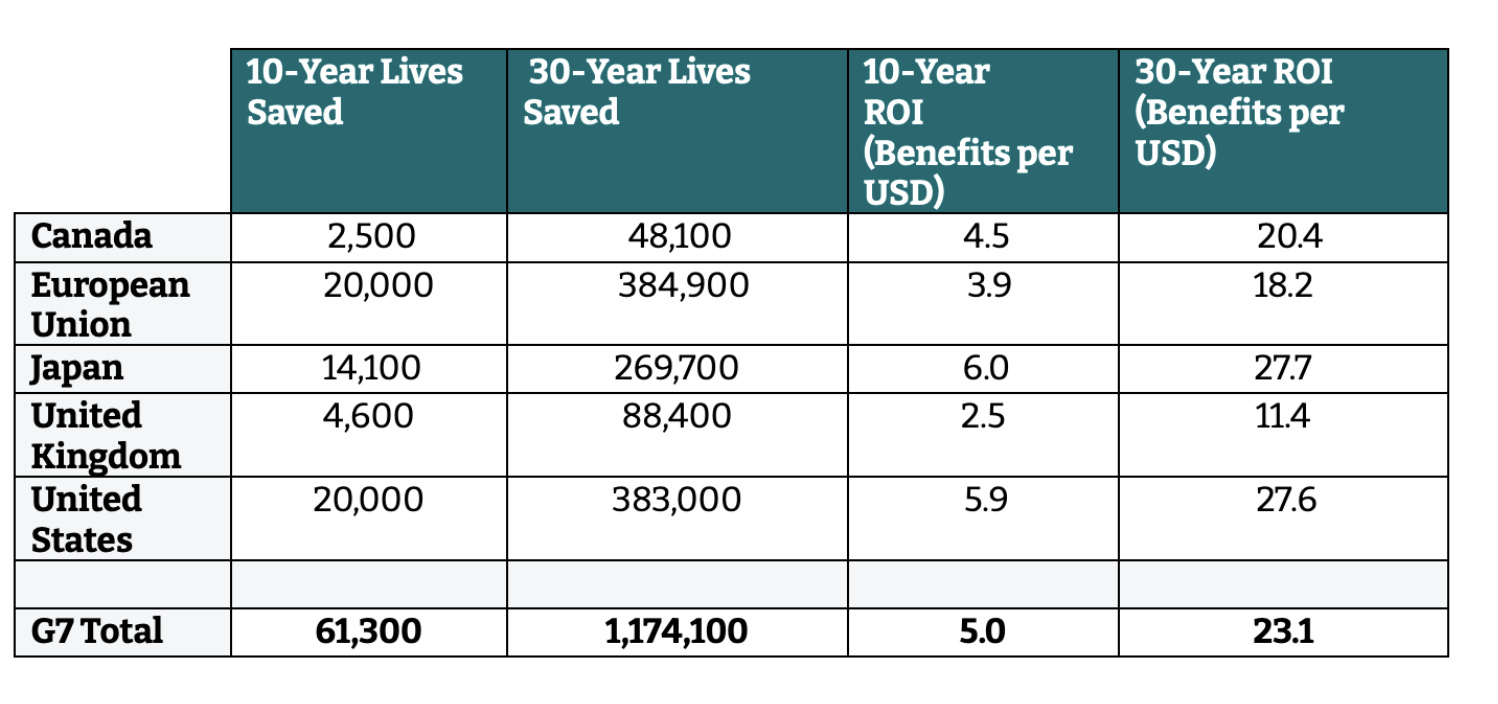
Despite these differences, we find that an antibiotic incentive program pays off for every G7 member country. ROI in the short term (10 years) varies from 2.5:1 (for the UK) to 6:1 (for Japan and the US). ROI in the long term (30 years) varies from 11:1 (for the UK) to 28:1 (for Japan and the US). Across the G7, the program would save 61,000 lives in the next 10 years, and 1.17 million lives over the full 30-year duration.
Table 4. Return on investment, by G7 member
Different countries, a common purpose
You can dig into our estimates in the full briefs here for Canada, the EU, Japan, and the UK, plus our original paper on the US. The details are wonky, but the message is clear: new antibiotics are a terrific investment for all G7 members—and we look forward to Japan’s leadership under its G7 Presidency to make this vision a reality.
Excel model available here.