This is a joint posting with David Wendt
The PEPFAR reauthorization bill, now signed by President Bush, is historic for several reasons. In our
last blog we addressed the implicit entitlements to treatment confirmed by this bill. Today we discuss the role that unit cost measurement is mandated to play in determining the targets set for future administration performance.
This may be the first time in history that any government has mandated performance targets based on estimates of the unit costs of meeting those targets. The language of the bill says: "the treatment goal...shall be increased...by the same percentage that the average US Government cost per patient...has decreased ..." [
Sec 403(3)(d)(3)].
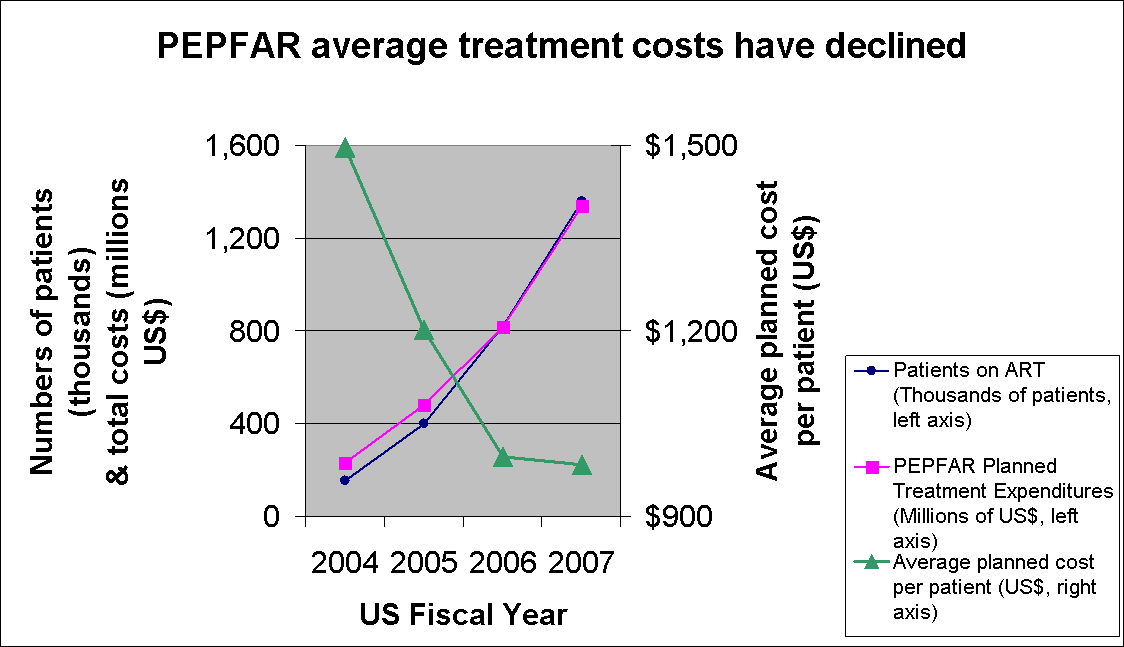
This is an interesting and innovative way to reconcile the objective of making foreign assistance more accountable (specific targets) with the recognition that unit costs of treatment are likely to vary over time. The chart below graphs the data on total planned treatment expenditure and the number of patients reported to be on treatment from 2004 through 2007 and shows that the number of patients (the blue line) has risen somewhat more rapidly than the total planned expenditure (red line).
If we define average costs as total planned costs divided by number of realized patients, average costs per patient (represented by the green line in the figure) declined by 40 percent from 2004 to 2007. Perhaps because of this trend, the language of the bill anticipates further reductions in the average costs and requires the government to increase its targets accordingly. This is really "average planned expenditure per patient enrolled" rather than "average cost per patient year," but lacking any data from OGAC on which to estimate what treatment actually costs, this approximation is a good place to start.
But the formula in the bill ignores that those who implement PEPFAR's treatment component, including Washington staff of OGAC, country-level U.S. staff, partners in the U.S. private sector and partners in the 15 host focus countries, can themselves influence unit costs. Some of those partners have an interest in increasing the efficiency of service delivery so as to reach more patients, others do not.
Increasing efficiency means working harder while receiving less per patient, so some partners will have the opposite incentive. Why work harder for less per patient when by making no effort to reduce average cost you can retain your current rhythm of work and your earnings? Altruism will motivate people to work harder, but self-interest pulls in the other direction.
In recognition of the potential pliability of average cost estimates in response to the incentives in the bill, the bill's authors added another innovative provision: they have said that: "Not later than September 30, 2009 and annually thereafter…Global AIDS Coordinator shall complete a study of treatment providers that…estimates the per-patient cost of antiretroviral HIV/AIDS treatment."
Wow! While there may be precedents for such a mandate imposed on domestic government agencies like Health and Human Services (can any of you readers cite a specific precedent?), I know of no precedent for this mandate in the area of foreign policy. Research institutes throughout the U.S. and beyond are probably already holding meetings to plan proposal writing in response to this mandate.
But the task will not be easy. The language of the bill recognizes some of the difficulties by asking that average cost estimates be computed "in specific categories of service providers, including urban and rural," etc. But the problem runs deeper. Studies have revealed that the average cost of service provision depends on the incentives to those delivering the service, not just on external factors. A research project called the PANCEA project (see
here and
here), on which I am a co-investigator, has found as much as 100-fold differences in average cost for the same service, only part of which can be explained by differences in types of providers.
And there's an even bigger issue - the possibility that sustaining and improving the quality of treatment will force an increase in average costs. What if the cost of maintaining a patient's adherence grows over time due to increasing toxicity of the drugs, or simple weariness of the patient? What if newly recruited patients require more adherence support than the "early adopters" who have so far been recruited? What if treatment programs are asked to assume the burden of more expensive second line treatment as
time goes on? What if treatment programs are increasingly tasked with other objectives, such as improving the general performance of the health sector or reaching out to prevent new infections in the community at large as I suggest should be asked of treatment programs in my recent
working paper? Then average costs per patient will rise rather than fall. The formula in the bill makes no allowance for this possibility. So the result of the formula is to penalize those who implement PEPFAR programs if they attempt to assume these additional, quality-enhancing costs. Although an innovative response to a real need, the formula will have to be revisited in order to avoid handicapping PEPFAR as it strives to sustain and improve the quality of its treatment programs.






