Recommended
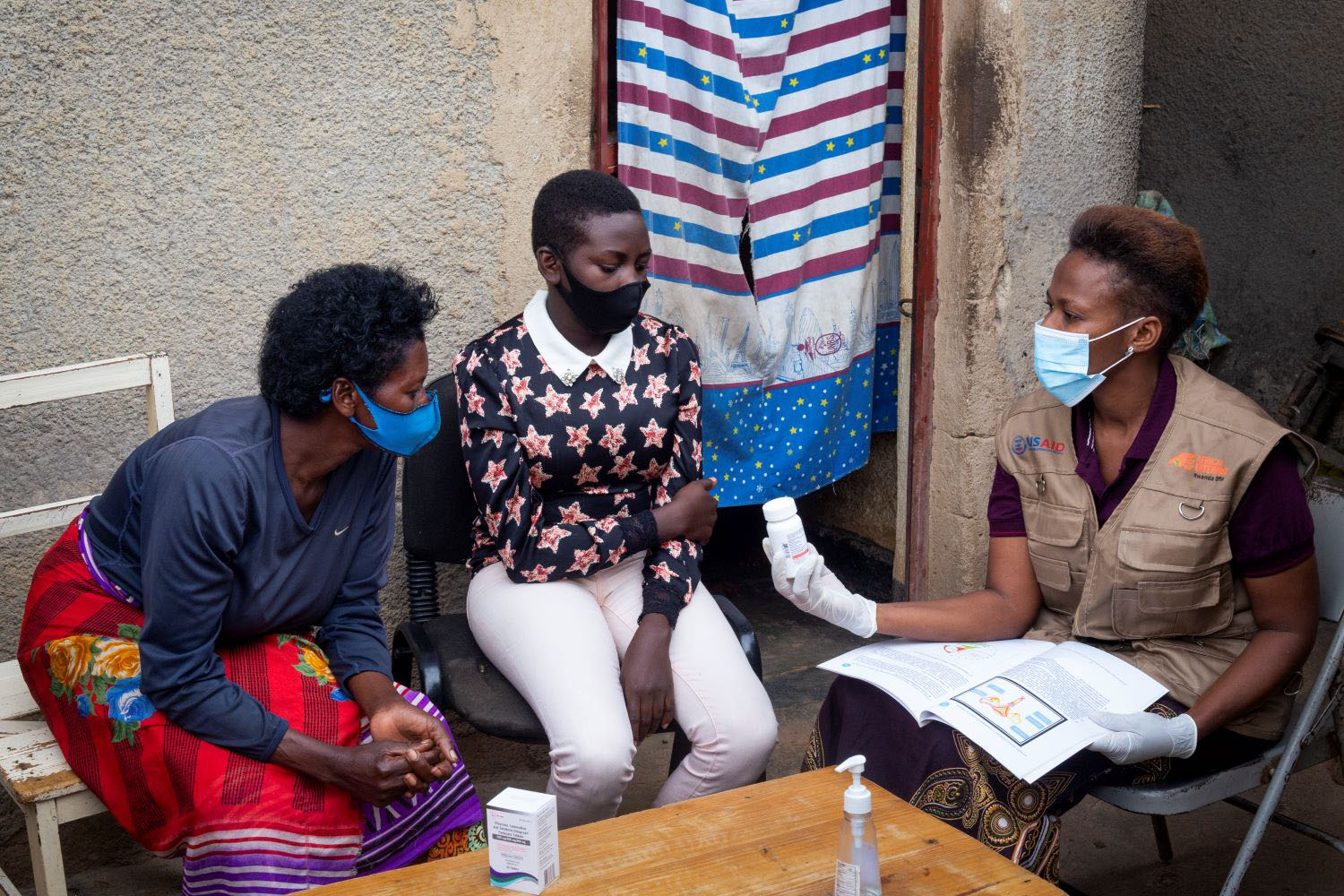
As countries strive to achieve the Sustainable Development Goals, including attaining and sustaining universal health coverage, decision-makers are increasingly using economic evaluation to drive macro policy choices and more granular technology-focused decisions. In a recent study, we discuss what cost-effective analysis (CEA) and benefit-cost analysis (BCA) have in common and where they differ, especially in relation to universal health coverage, in terms of the perspective of the analysis and how the methodologies relate (or not) to the viewpoints of healthcare policymakers and budget holders in low- and middle-income countries (LMICs).
Here we tackle the question of when and for what sort of decisions policy-makers should use CEA as opposed to BCA. We conclude that the two approaches are complementary and can add value, when applied correctly, to national and subnational healthcare budget holders keen to enhance access to good value services and technologies.
Context matters
The answer to the question of when CEA or BCA is the more appropriate approach lies in the nature of the opportunity cost of decisions. In allocating a budget for healthcare (“within-sector allocation”), CEA is preferable. For decisions regarding the size of that budget (“cross-sector allocation”)—and therefore the wider value of resources for other public or private sector uses—BCA is preferable. This distinction stands irrespective of the perspective of a study. It is commonly thought that a study from a societal perspective ought to use BCA, but this is so only if there are significant opportunity costs or incidental impacts outside the health sector which would require monetisation for comparison with gains or losses within the health sector. A study from the societal perspective where costs and benefits accrued within the sector need not be wider than a CEA (with distributional analysis over time and populations as appropriate).
In an environment where resources are scarce (and this includes rich and poorer settings alike), economics suggests that decisions should be based on opportunity cost: investments should be made only if the value thereby obtained exceeds the value of the activity displaced. For example, CVS Health recently announced it would use CEA to inform how it compiles it medicines list, triggering a backlash from Big Pharma. Although most people would readily agree that value matters when deciding what to pay for in more or less every setting, there is less agreement on how that value is best expressed (for further discussion on value in the US setting, see here). Our argument is that, whatever its form, the value must exceed its opportunity cost. Opportunity cost critically depends on the range of opportunities available. These, in turn, are dependant on whether the options are essentially only within the sector or also lie outside it.
The method of valuation required is different in the within-sector and cross-sector allocation contexts. Granted that the principal output of universal health coverage is couched in terms of population health and its distribution, choices within the healthcare budget have an opportunity cost also in terms of population health and its distribution: the measure used for outcomes (life-years, DALYs averted, QALYs, etc.) can therefore also be used for opportunity costs. In choosing between alternative possible budgets for healthcare—and therefore between health and outcomes in other sectors, such as education or transportation—this metric will not do: the preferred approach is to assign dollar values to both the health outcomes (life-years, etc.) and the multitude of other possible non-health outcomes (e.g., improvements in transportation systems).
BCA examples
In the UK, Lord Layard’s proposal for large scale expansion of psychotherapy is an example of economic analysis that was used for investing general taxation revenue prior to it being allocated to any specific purpose. Lord Layard used a BCA approach to make a case directly to the UK’s treasury and prime minister’s office for new centrally allocated funds rather than from the existing NHS allocation. One should note that this misuses CBA—there may well have been better uses for additional resources for health care in the UK than psychotherapy, which would have been revealed had both a CEA and a BCA been conducted, illustrating a case where the two are complementary.
In LMIC settings, presenting policymakers with BCA including favourable cost benefit ratios triggered investment in wheat fortification in Haiti and in electronic procurement infrastructure in Bangladesh.
The distinction is essentially pragmatic, and where it is tenable, it carries the great advantage for decisions in the health sector of not needing research-intensive (and itself costly) efforts to derive monetary values for health gains and losses, and not entering the ethical quagmire concerning the acceptability of monetising health.
For allocating budgets across sectors, a multitool approach is best
For decision-making about general tax revenues, the concept of opportunity cost is a lot harder to translate into an operationalisable threshold as the marginal dollar, pound, euro, or baht could be spent on roads, welfare, education, defence, or debt reduction, or be handed back to the tax-paying public as a tax cut. Indeed, it is hard to think of any practicable and uncontested measure which could be used to evaluate and compare investments across all these different sectors other than the revealed monetary value of their outcomes and where precedent and political priorities rather than evidence, may take precedence. This challenge for BCA does not, however, remove the requirement to prove that, in Lord Layard’s case, psychotherapy was indeed the best (at least in terms of health outcomes) use of additional healthcare resources compared to other possible healthcare investments. To make such a case, one would have to carry out a within-sector CEA before the BCA.
Cross-sector allocation decisions demand evaluative approaches and an evidence base that enables comparisons of outcome and opportunity cost of comparable scope and quality in all the different sectors in question. While important gaps remain, arguably the methods and data available for the assessment of health services is very much advanced relative to sectors such as defence, education, and criminal justice, where the dimensions requiring monetary valuation are significant and complicated (e.g., deterrence in defence, educational attainment and non-commercial human capital in education, reduced social isolation in housing services) and there is a long way to go systematically to measure the impact on interventions on such dimensions, let alone to assign dollar values to them. While attempts have been made to address this comparative lack of evidence, such as the establishment in the UK of “What Works” centres and Pew’s clearinghouse, right now there are no credible and relevant outcome measures that can be used outside the health sector. In most instances, basic research and data collection are needed to start building an evidence base for value-for-money assessments of any sort.
So, a more pragmatic approach may be initially to focus on within-sector evaluations using measures of effectiveness for which data can be gathered and supplemented with qualitative evidence, and, as in health, building institutional structures that can translate values, political judgement, and evidence into policy.
For allocating funds within the health sector, CEA is the right tool
The situation is different when it comes to allocating within-sector scarce healthcare budgets across disease and conditions, interventions, and populations. In that case, CEA/cost utility analysis are the right tools for making allocation decisions. CEA, especially when its results are expressed in the form of net benefit, can reflect empirically and context-sensitive opportunity costs of alternative investments in healthcare services and technologies, and hence inform the design and adjustment of health benefits packages, core components of delivering on the UHC promise. (See here, here, here, and here for examples of such processes.) To achieve this, it is critical that the decision rules for judging whether an intervention of a given incremental cost-effectiveness ratio is cost effective are informed by locally relevant estimates of opportunity costs. Recent work on empirically deriving opportunity costs in high-income countries (Canada, Norway, and the UK) and LMICs makes this increasingly possible. Further work that proposes a multisectoral approach to measuring the opportunity cost of investments beyond health within a CEA are also in development (e.g., see here), with a view to informing how CEA is used to help allocate resources in the UK’s National Health Service (see appendix B in this study).
As argued by colleagues of ours in response to a call for using “real economics” (AKA economics consistent with normative welfarist principles):
If the needs of decision making are paramount, the objectives and constraints of those made responsible for resource allocation cannot be ignored. This includes absolute clarity about the centrality of a threshold representing opportunity costs, regardless of how health is characterised and whether or not studies are defined as CBA or CEA.
Political discourse has become more sceptical of, and indeed hostile to, evidence-based decision-making in the last few years. This environment should remind economic analysis practitioners of all persuasions of the values they share and the importance of working constructively together. It is sometimes said, allegedly quoting Henry Kissinger, that there are so many arguments in academia because the stakes are so small. When it comes to the economic analysis of global health, we do not have that excuse.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.