Recommended

Blog Post
ODA Rules Must Ensure Vaccine Donations Count for Poor
Vaccine inequality is rampant. Someone in a high-income country is 11 times more likely to have been fully inoculated than someone in a low-income country. Whilst more than a third of those in high-income countries have received a booster shot, only 10 percent of those in low-income countries have received their first dose. The disparities are truly shocking: these countries need vaccines.
In this context anyone stockpiling vaccines to sell at a profit on the secondary market would likely be labeled a profiteer, and not the jovial, sympathetic kind so beloved of British sitcom writers. But unless something changes, this is exactly what the UK government is poised to do. The continued absurdity of the Organisation for Economic Co-operation and Development (OECD)’s rules for counting official development assistance (ODA) is colliding with the Treasury’s obsession with minimising the government’s outlay on helping other countries, despite the fact that this goes against the opinion of MPs across the political spectrum.
Most OECD countries are now pushing to count donations of COVID-19 vaccines towards their aid, with the current proposal that each vaccine donated being counted as equivalent to $6.72 of ODA, regardless of how much the vaccine actually costs. This figure is the average price COVAX has paid for vaccinations, including the cost of delivery. While for some countries, the vaccines they procured and plan to donate cost much more than this $6.72 compromise cost (meaning they are giving away vaccines at a discount of sorts), the UK paid much less. Coupled with the government’s promise to count “all ODA eligible spend” towards the UK’s aid target, this amounts to making a (fiscal) profit on vaccines being given away. The UK spent around $4.40 per vaccine to be donated. So, if it counts them at the OECD’s $6.72 price, the government will cut $2.32 from the rest of the aid budget per vaccine donated. Any generosity we show with vaccines will be more than offset by cuts elsewhere, while the Treasury gets to have its cake and eat it, claiming to meet the 0.5 percent target while spending even less than this reduced amount.
We think this is wrong, and a recent poll of Parliamentarians that we commissioned from YouGov shows that MPs across the political spectrum think so too.
We set out below how the OECD plans to count COVID vaccines, why this reduces the UK’s overall spending on ODA, and how MPs think we should actually count the vaccines.
How countries are looking to change the rules
The OECD Development Assistance Committee (DAC)’s current proposal is to count vaccines at the average price paid by COVAX. They present several arguments for this, none of which are compelling.
- First, they note that usual practice is to record aid-in-kind “at prevailing international or national market prices”, instead of the price originally paid for the goods. This makes sense for standard commodities such as parcels of food, but vaccine doses do not have a prevailing market price, and differ in the protection they offer and how they are delivered, so it makes little sense to treat them as standardised.
- Second, they rightly point out that the original prices paid for doses are confidential and are therefore unverifiable. But it would be a remarkable indictment if the DAC were setting rules on the basis that members couldn’t be trusted to be honest, and in any case, they could have opted to value doses at the average price for each type of vaccine (as per earlier proposals) which would be closer to the original prices paid. Given that most doses donated will likely be the cheaper vector vaccines, using the average will systematically overstate the fiscal effort of DAC members.
- Finally, they highlight the risk that setting a price too low could incentivise countries to sell, rather than donate vaccines. But this risk seems overblown: the constraint on selling is more reputational than fiscal, and there may be few willing buyers given most ODA-eligible countries are eligible to receive vaccines from COVAX for free (if they would rather buy, this would suggest deeper problems with how COVAX operates).
Instead, the choice to value donated doses at the average price paid by COVAX likely reflects internal dynamics in DAC discussions. The DAC is a consensus-based organisation, whose decisions often seem more based on political self-interest than technocratic concerns. As such, it is much easier to form a consensus around rules that increase reportable ODA, and these ultimately prevail. The valuation of vaccine donations is a case in point.
Initially, the DAC was primarily concerned with avoiding ODA inflation or diversion, and made a convincing argument that donating excess vaccines shouldn’t count at all (because it represents an “ex post decision by the donors, with no original intent to benefit developing countries”). Fast forward a few months, and the proposed price is more than double the original, and the concern is with the perverse incentives of valuing donated vaccines too low. And while the average cost of $6.72 is based on GAVI’s “fully-loaded” estimates, including costs of shipment and syringes (para 13), the latest proposal also indicates that donors can count these ancillary costs separately. The proposal has not yet been accepted: the US and the Netherlands continued to object to the inclusion of donated vaccines in ODA. But it is likely a matter of time. Both have signaled willingness to let the proposal pass despite their misgivings. But it is striking how starkly their stance contrasts with the intention of the UK: to exploit the leniency of the rules to the full, to reduce its ODA expenditure.
The UK essentially makes a profit for every vaccine donated
Different COVID vaccines have different prices, and the price for the same vaccine can vary considerably based on how many a country is buying and when they negotiated their purchase. It is also difficult to find public information on which vaccines countries are donating. However, information from the House of Lords shows that as of December 7th the only vaccine the UK had donated to low- and middle- income countries was AstraZeneca’s. These donations make up only 16 percent of the pledge the UK made at the G7 to donate 100 million vaccines by June 2022. We have been told that ultimately the UK government expects to donate all 20 million of Janssen’s vaccines it has procured, with the rest coming from AstraZeneca.
Whilst the price the UK pays is not public knowledge, it is thought to be about the same as the roughly $3 the EU has paid, as shown on UNICEF’s dashboard. This dashboard also lists the EU as paying $8.50 for Janssen’s vaccine, and other purchasers as paying $10. If the UK pays the higher figure for Janssen that would suggest that as of December 7th it has paid about $3 for every vaccine donation, but that average cost would rise to $4.40 once the 100 million pledge was reached. Under proposed DAC rules however, the UK could claim that the value of the donations it had made were $6.72. Given the 0.5 percent spending the UK has committed itself to, in practice the UK would thus cut funding for other programs by $6.72 and reduce its overall aid spending by $2.32 per donation, meaning that there will be a $232 million reduction in UK’s actual ODA—roughly equivalent to the UK’s entire 2020 bilateral allocation to Uganda and the Tanzania combined.
The British government originally purchased these vaccines not with the aim of helping people in less well-off countries, but because it wanted the option to distribute them to its own population. Now that the NHS does not need these doses, giving them to poorer countries makes sense. As well as being the right thing to do, it is in the UK’s interest to reduce infection across the world to stop new variants from spreading.
We've previously argued that it would make sense not to count vaccines as ODA at all; charging significantly more to ODA than we ever spent on them, as seems likely, is nonsensical and perverse. And it’s not just development-focused people who believe so.
Polling data suggests MPs agree with us
In December 2021, we partnered with YouGov to poll a representative sample of MPs about a host of issues relating to the UK’s aid budget and development policy (stay tuned for more from that work). One of the questions we asked was about how the UK should count surplus COVID-19 vaccines as ODA. The results are rather striking:
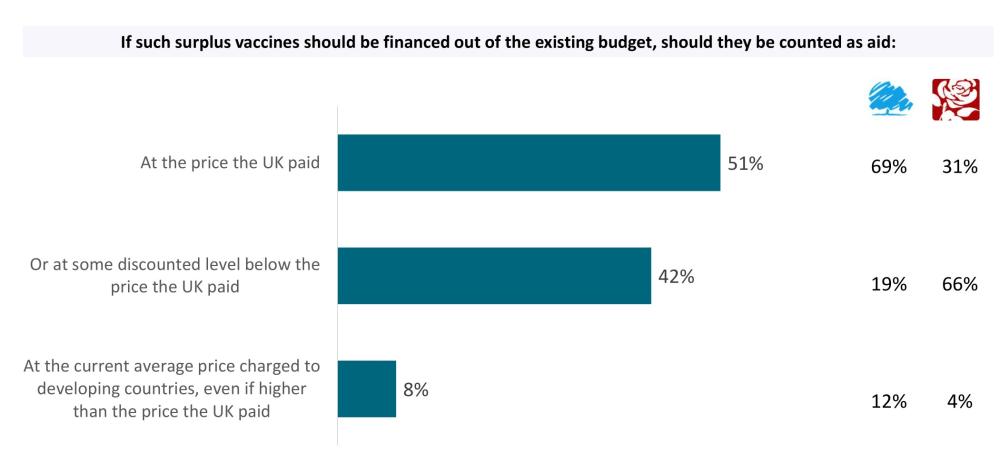
Figure: Most MPs think vaccines should not count for more ODA than the UK paid for them
Source: YouGov poll on behalf of CGD; poll conducted in December 2021, on a sample of 88 MPs, representative by party, gender, electoral cohort and geography
Both Conservative and Labour MPs in our sample overwhelmingly report that they believe we should claim—at most—the price paid for the vaccine as ODA. Fewer than a tenth of MPs select an option which gives the possibility of claiming more ODA than the price we actually paid.
If using the OECD’s proposed "ODA price" for vaccines is bad for development, unpopular with MPs, and against the spirit in which the ODA statistics are calculated, the UK shouldn’t do it. It should—voluntarily, regardless of what the final OECD rule chosen is—opt not to claim ODA for the surplus vaccines it donates to poor countries. And if this is a step too far for the Treasury, it should at least commit to not claiming more than we originally spent. Any other decision would be illogical, immoral, and unpopular.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.