Recommended
Even before the COVID-19 pandemic broke out, the quality of health services across many African countries was too low. Various research documents different aspects of this. Some studies highlight insufficient medicines or equipment. Some focus on health worker knowledge. Others highlight high levels of absenteeism or low levels of effort by health workers. While each of these ingredients of the health system is important, examining them one-by-one gives a limited picture of whether health facilities are ready to provide care.
The Service Delivery Indicators (SDI), a data collection initiative from the World Bank, the African Economic Research Consortium, and the African Development Bank, provide a novel opportunity to examine whether health workers are present in primary and secondary care facilities, whether they know enough to diagnose and treat common ailments, and whether they have the equipment and medicines available to do so. The SDI are nationally representative surveys of health facilities and schools. In health facilities, the SDI use clinical vignettes to assess health worker knowledge, unannounced visits to assess absenteeism, and visual inspections to assess the availability of medicine and equipment. SDI health survey data are currently available from ten countries in Africa (download them here): Kenya, Madagascar, Mozambique, Niger, Nigeria, Senegal, Sierra Leone, Tanzania, Togo, and Uganda.
In an article that is now forthcoming at BMJ Global Health, we draw on data for more than 20,000 health providers and 8,000 facilities to construct an aggregate measure of heath care readiness. If a patient shows up at the health facility with a common condition (like malaria or diarrhea), what is the probability that there is a health worker present with the knowledge to diagnose the condition correctly and prescribe the appropriate treatment, as well as the medicine or equipment she needs to do so? (The math on how we build the measure is in the paper.)
What do we find?
Diagnostic and treatment accuracy
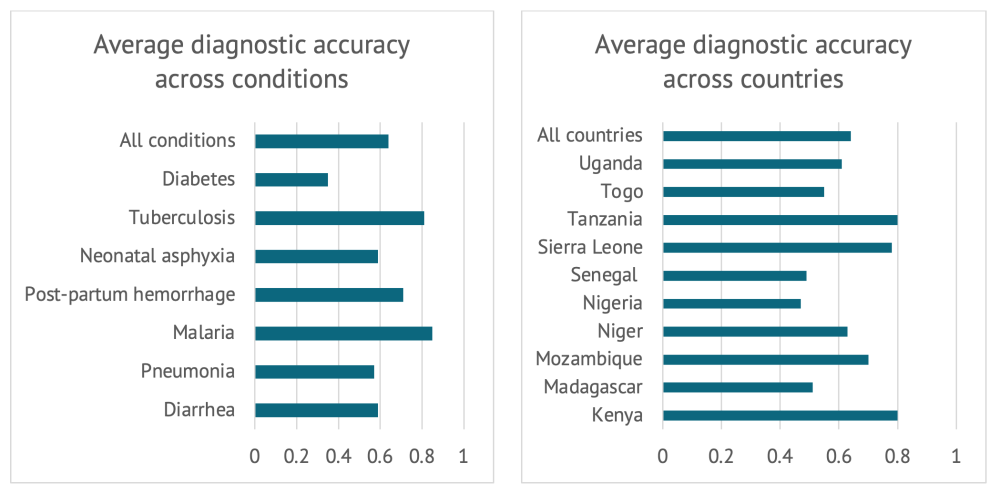
How accurately do health workers diagnose common conditions? Across the seven conditions that the SDI evaluate using vignettes—malaria, pneumonia, diarrhea, tuberculosis, diabetes, post-partum hemorrhage, and neonatal asphyxia—health care workers correctly diagnose just under two-thirds of cases (64 percent—see the figure below). Diagnostic accuracy is lowest for diabetes (35 percent) and highest for malaria (85 percent). Of course, there is wide variation both across countries and within countries: 18 percent of workers correctly diagnosed diarrhea in Madagascar versus 95 percent in Sierra Leone. Keep in mind that this does not reflect a failing on the part of health workers. Health workers were hired, trained, and certified for a job by a health system. It’s a health system’s job to make sure its workers have the knowledge they need to do their job well.
Figure 1. Diagnostic accuracy across conditions and countries
Source: Di Giorgio et al. 2020
Once health workers have diagnosed a condition, how likely are they to prescribe the correct treatment? After a correct diagnosis, health workers recommended a correct treatment in 72 percent of cases. If you take the two together—what are the chances of a correct diagnosis and treatment—the number falls to 45 percent.
Health worker absenteeism
Yes, providers need to be able to diagnose and prescribe treatments for patients, but to do either of those things, they have to be present in the first place. The SDI show large variation in absenteeism across countries. The average absenteeism across all countries—of doctors and nurses who are on the roster as being on duty at the facility when the enumerator shows up unannounced—is 30 percent, but it’s much lower in some places than others: just 16 percent in Tanzania and a full 50 percent in Togo.
Drugs and equipment
When we look at the availability of four essential drugs—for treatment of malaria, diarrhea, pneumonia, and postpartum hemorrhage—we find that only 42 percent of facilities have all four. In Uganda, that number is at its lowest, at 14 percent. In Nigeria, it’s 21 percent. 70 percent of facilities across all countries had a minimum set of medical equipment.
Overall health care readiness
If we take four conditions important for maternal and child health, just 14 percent of facilities across the ten countries have at least one provider present and able to correctly diagnose and treat diarrhea, pneumonia, post-partum hemorrhage, and neonatal asphyxia, with the minimum drugs accessible. If we just focus on child health or maternal and neonatal health, that number rises to a still-troubling 28 or 29 percent.
What if facility conditions were different?
What if health worker absenteeism were zero? What if all the necessary drugs were available? We simulate how much care readiness would improve under these conditions. It does get better, to be sure, but not by as much as you might think. Under either of these hypothetical conditions, care readiness for maternal and child health conditions remains under 20 percent (up from 14 percent). Why? Providers don’t demonstrate the knowledge they need to diagnose and treat cases.
In fact, this picture is still too rosy. While the SDI data can effectively capture what health providers know, whether they’re present, and what materials they have to work with, they still don’t capture what providers actually do. We have evidence from multiple studies, including standardized care studies where an actor poses as a patient and—unbeknownst to the doctor—evaluates the quality of care, which show there is an additional care readiness gap beyond what we observe in our data.
Conclusion
This analysis demonstrates that improving health worker knowledge must be a top priority for health systems. Training programs have shown mixed results, so what that probably looks like is a combination of better training—both pre-service and in-service—along with better hiring and working conditions that attract bright candidates. In the absence of health provider know-how, there are limits to what other improvements will deliver.
Topics
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.