Recommended

REPORT
Collecting Evidence to Inform COVID-19 Vaccine Procurement Decisions
Blog Post
Who Gets a COVID-19 Vaccine and Who Pays? The Need for Economic Analysis

Event
Economic and Programmatic Implications for the Covid-19 Vaccine Roll Out in Africa
VIRTUAL
October 28, 2021 7:30—9:00 AM Eastern Time (US and Canada)COVID-19 vaccine access is a critical issue of our times, and both international institutions and wealthy countries are falling short of the often-used rhetoric on achieving vaccine equity.
COVAX, a joint initiative from several UN organisations to facilitate equitable access to COVID-19 vaccines, expects to miss its target to distribute two billion doses by the end of 2021 by nearly a third. Additionally, even though substantial bilateral donations have been pledged, only a small fraction of the doses promised have been delivered.
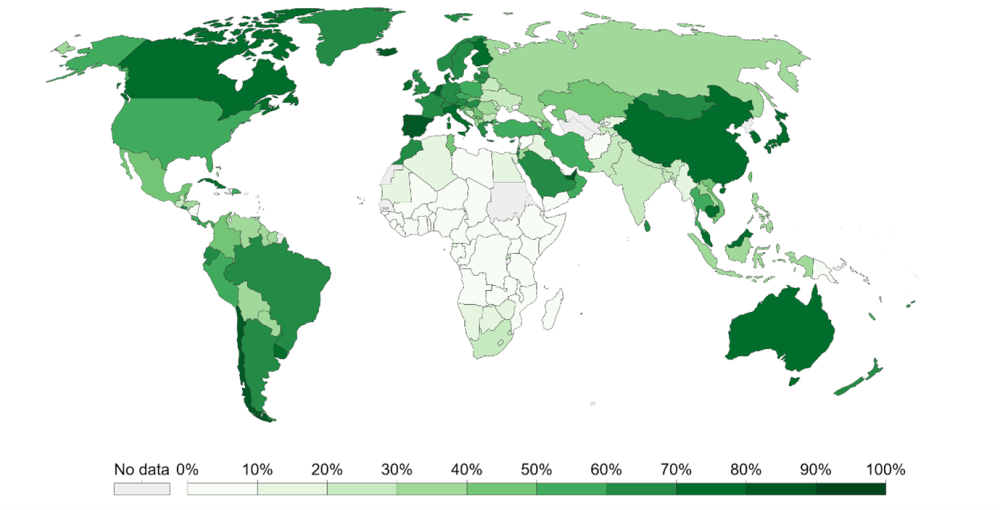
At the time of writing, the majority of African countries have fully vaccinated less that 5 percent of their populations, compared with over 80 percent in leading countries and a world average of 38 percent (see Figure 1). There is still a long way to achieve the goal set by the African Centres for Disease Control and prevention to work with their member states toward vaccinating a target of 60 percent of their population.
Figure 1. Share of the population fully vaccinated against COVID-19
Source: Official data collected by Our World in Data – Last updated 23 November 2021
To complement those donations, African countries are procuring COVID-19 vaccines directly through the Africa Union’s Africa Vaccine Acquisition Trust (AVAT) or are pursuing bilateral agreements with manufacturers.
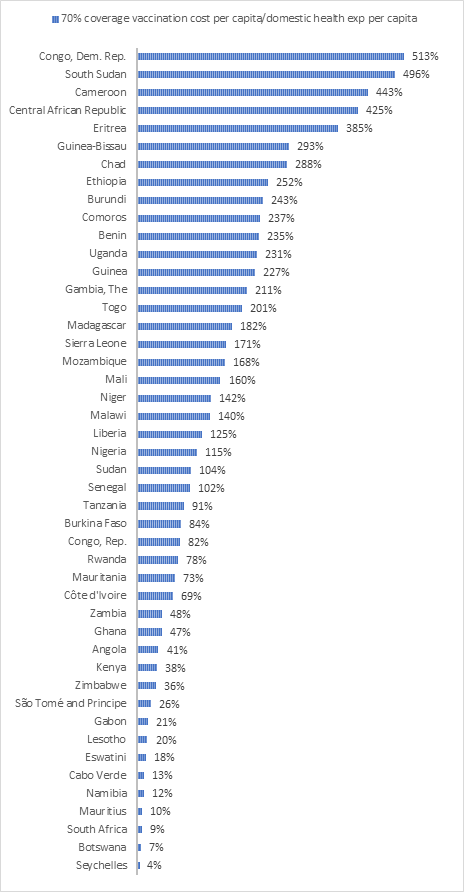
However, in many countries (especially in low-income countries), achieving high levels of coverage would be costly. For instance, calculations of the cost of vaccination per capita expressed as a proportion of total government health expenditure per capita have shown the significant budget impact of vaccination campaigns. In over half of African countries where those estimates are available, the cost of vaccination exceeds the total government health expenditure (53 percent or 25/54). In South Sudan, Cameroon and the Central African Republic, the cost would be equivalent to 4 to 5 times the total government health spending per capita. In such low resourced settings, the financing of essential health services could easily be jeopardised by COVID-19 vaccine deals.
Figure 2. Vaccination cost per capita as a proportion of total government health expenditure
Source: World Bank Blog - Calculating Sub-Saharan Africa’s COVID-19 vaccination financing gap (May 2021)
Given the above, how much COVID-19 vaccine should African countries buy? Which, of the now many, vaccines offer the best value for money? How does vaccine price and affordability affect both questions?
Evidence can help—CGD has teamed up with Africa CDC to develop a toolkit
The International Decision Support Initiative and the Africa CDC Health Economics Unit have developed a toolkit for collecting evidence to support COVID-19 vaccine policy making.
What the toolkit does:
-
Summarises what Health Technology Assessment (HTA) is and why it may be a helpful framework to support evidence collection and decision making.
HTA is a framework to support the use of wide-ranging evidence when policy makers are faced with a decision on whether to spend public finance on a health technology (or service). HTA has supported public payers making decisions on procurement of health technologies, including vaccines, for decades now; and the practice is gaining momentum in the African region. -
Identifies four categories of evidence they may be valuable to decision makers: Supply and Logistical Constraints; Ethics and Equity; Value for Money (costs against direct and indirect benefits); and Budget Impact.
-
Within each category of evidence, provides a summary of potential considerations, methods for analysis and links to key resources.
What the toolkit does not do:
-
Provide general recommendations on policy.
-
Replace the need for evidence collection and appraisal.
-
Replace the need to a local policy process and legitimate decision making.
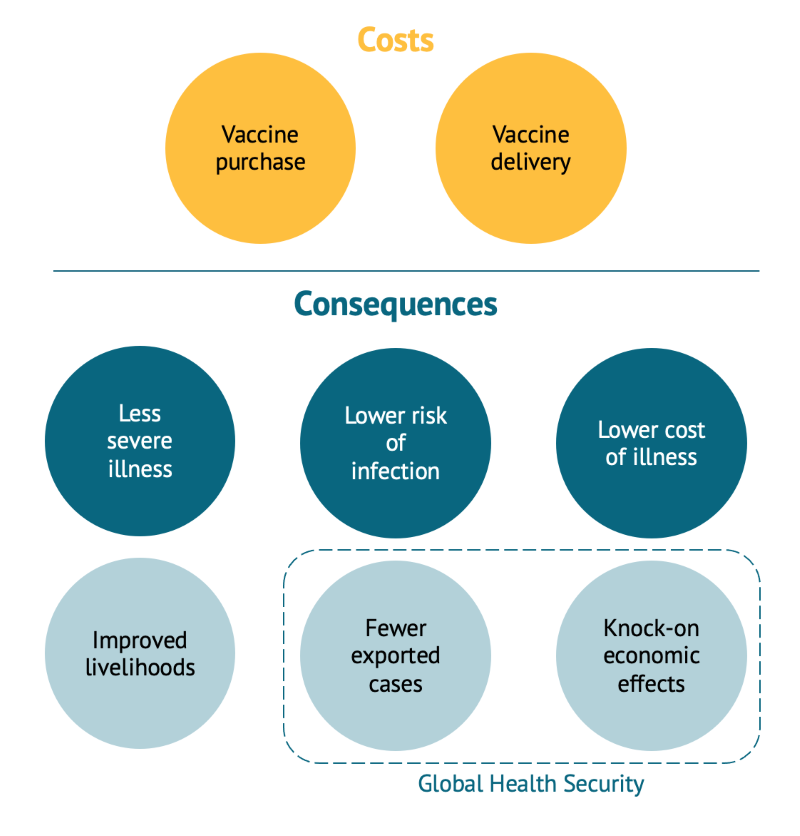
The elephant in the room: global health security
While most categories within the toolkit consider the value of vaccination from a national perspective, the toolkit makes the case for considering the benefits of controlling widespread SARS-CoV-2 in the rest of the world, including high income countries as well. These benefits of disease control are associated with reducing the likelihood of imported infections and novel strains, as well as economic risks to supply chains linked to depressed international trade.
Conclusion
We hope this toolkit supports decision makers in African countries make the challenging and highly consequential decisions associated with COVID-19 vaccines procurement. We also hope it conveys an important message for leaders in high income countries: low-income countries cannot finance high levels of COVID-19 vaccine coverage without jeopardising essential services and the benefits of increased vaccine coverage will extend well beyond Africa.
Topics
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.