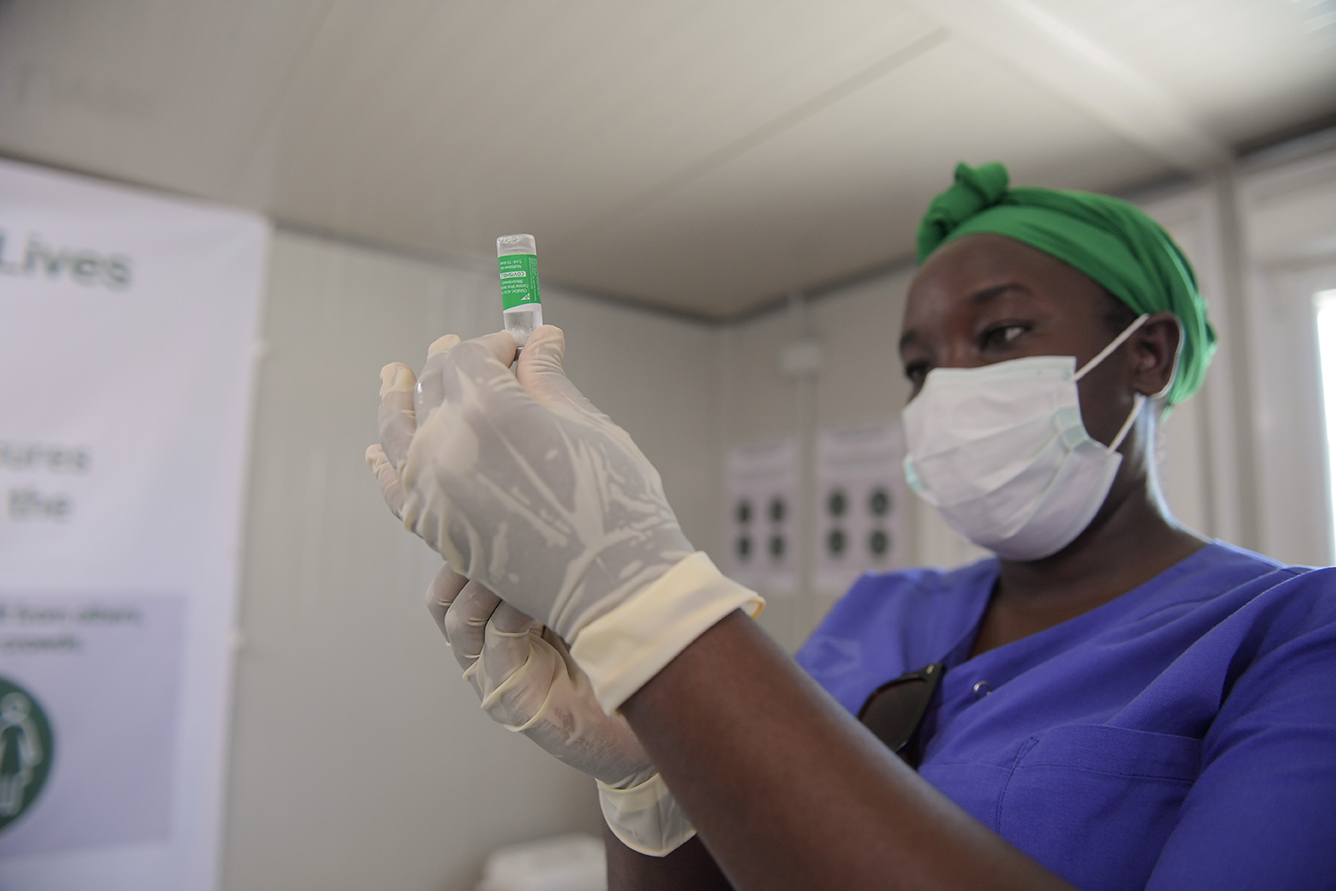
As the most fragile Americans line up for a dwindling supply of flu shots, many people are wondering why vaccines, arguably the most essential and cost-effective pharmaceutical products, seem to be one of the health system’s weakest links. Americans are discovering what people in the developing world have long known: on their own, markets fail to provide the right vaccines when and where they are needed most.
This is big problem with a clear solution. Large purchasers, like governments, could promise to buy safe, effective vaccines at prices high enough to permit a reasonable profit. Such an arrangement could have greatly lessened the flu shot shortage. Offering similar guarantees for vaccines that don’t yet exist would unleash the competition of the marketplace to combat some of the world’s worst diseases.
Think of it as a medical version of the $10 million prize recently awarded for the first privately financed passenger craft to reach sub-orbital space twice in two weeks. Just as the Ansari X prize jump-started space tourism by creating a race to space among private firms, credible promises to buy vaccines at prices that ensure a fair profit could spark a race for the creation of life-saving immunizations.
Developing countries have made good use of vaccines originally created for rich countries. Three quarters of the world's children are vaccinated for polio, whooping cough and diphtheria – saving 3 million lives a year. At least 7 million more lives could be saved if vaccines existed for malaria, AIDS, TB and other diseases devastating the poorest countries.
But under current rules, pharmaceutical companies – the engines of innovation in modern medicine – lack incentives to invest in vaccine R&D and production. Small markets are part of the problem: vaccines make up less than two percent of the $340 billion global pharmaceutical market, so they are not high on investors’ priority lists. The developing country vaccine market is even smaller: a mere $500 million or about one-tenth of a percent of annual global pharmaceutical sales.
Then, too, vaccines are much riskier to develop and manufacture than compounded chemical medicines and the regulatory requirements are especially stringent. Add the bad press that comes with every alleged adverse reaction, plus companies’ fears that governments might nullify the patent on a successful vaccine or insist that they sell at money-losing prices, and it is no wonder that pharmaceutical executives say "no, thanks" or "next year, perhaps" to suggestions that they enter the vaccine business.
As a result, only a handful of big companies conduct research on new vaccines, compared to more than a dozen two decades ago. In the 1980s, seven firms in the U.S. were licensed to produce basic childhood vaccines; only three remain in the business today and these hesitate to invest substantially in R&D or expanded manufacturing. Overall, a mere 10 percent of R&D funding in health is devoted to finding vaccines or drugs for the diseases that make up 90 percent of death and disability in the world.
Public funding of basic research through the National Institutes of Health and other government agencies addresses part of the problem. And recently, philanthropy has spurred R&D on vaccines against neglected diseases. Just this month scientists at GlaxoSmithKline supported by a grant from the Bill and Melinda Gates Foundation announced favorable results from research on a malaria vaccine -- a breakthrough that may eventually prevent many of the 800,000 childhood deaths that occur in Africa each year.
But because research subsidies are limited, public and philanthropic funders must "pick a winner" early in the process, bypassing other promising approaches. For example, there are 25 other vaccine candidates for malaria; nobody knows which will be most effective in the end. A commitment to pay for an effective malaria vaccine would spur fresh research into neglected possibilities, as companies compete for the rewards of success.
Current rules will neither ensure a steady supply of the flu vaccine nor inspire innovations to prevent the diseases that plague the world’s poorest people. We can fix this by enlisting the power of markets. The price of failure will be paid in lives.
Ruth Levine is a Senior Fellow at the Center for Global Development and author of the forthcoming book Millions Saved: Proven Successes in Global Health.