Recommended
After months of devastating news about cuts to US global health programming, the Trump administration's America First Global Health Strategy presents some grounds for optimism. It signals continued US commitment to global health, including the delivery of lifesaving assistance, alongside containing outbreaks and preventing pandemics. However, it also proposes the rapid phase-out of support motivated by cost savings. Instead, we argue that US global health support—especially for HIV and malaria—should be based on sunsetting these infections as major killers worldwide—and not the few hundredths of a percent of US GNI that the administration spends fighting them.
It is welcome that—at least in the short term—the strategy promises to “ensure funding for 100% of all frontline commodity purchases and 100% of all frontline healthcare workers who directly deliver services to patients.” And as forecast by Rachel Bonnifield and Janeen Madan Keller, the strategy advances several positive policy directions. The emphasis on government-to-government mechanisms, integration across disease silos, and deeper collaboration with national health systems reflects a growing bipartisan consensus, echoing what has already been proposed in recent USAID and PEPFAR strategy documents. It makes absolute sense to integrate community health worker programs across disease-specific programs including HIV/AIDS, TB, malaria, polio as well as maternal health, to develop shared laboratory networks that serve multiple disease programs; and create unified health information systems. The strategy is also right to prioritize working as much within government systems as opposed to beside them. As the strategy points out, experience from Kenya and elsewhere suggests this can increase sustainability and quality while reducing costs. The focus on harnessing cutting-edge innovations like lenacapavir (an injection that prevents HIV infection) is also promising, helping to advance progress amidst a rapidly changing landscape.
A one-size-fits-most timeline and approach
Regarding transition, the strategy promises multi-year bilateral agreements with recipient countries involving clear benchmarks and co-investment requirements. This provides a structured framework that previous transition efforts have often lacked. But it also suggests that the US will “rapidly transition technical assistance from supporting individual clinical sites to supporting governments in taking over key functions” and that the “majority of 71 U.S.-supported countries will transition to full self-reliance during the term of the agreement.” Funding will not increase regardless of the unmet need for services and, starting in fiscal year 2027, the strategy suggests US assistance levels will decline. This is particularly concerning given that draft House legislation proposes a 50 percent overall reduction in global health spending by FY2028 (which starts two years from now).
We have learned from past experiences that premature withdrawal of support can quickly reverse hard-won gains. This can lead to increased morbidity and mortality and the potential spread of drug-resistant strains that threaten regional and global progress: it happened with early global progress against malaria and has dogged the fight to eradicate polio. And this year provides evidence of what can go wrong if transitions are poorly managed: the abrupt termination of USAID awards caused widespread service disruptions and deaths.
As noted by CGD colleagues, in poor, fragile, and conflict-affected settings, a full transition is not realistic in the short term. Consider the contrast between South Africa and Malawi. South Africa was already covering 90 percent of treatment costs and health spending for HIV/AIDS, with overall health spending of $570 per person per year. While that spending is still only five percent of the US level, it represents a fundamentally different context than Malawi, where health spending is $40 per person per year (or 0.3 percent of the US level). Moreover, in Malawi less than a quarter of healthcare providers demonstrate an ability to both diagnose and treat malaria with anaemia, and on average, health facilities had 10 of the 18 most basic pieces of equipment and supplies to deliver child healthcare. The transition to reliable service provision for even basic infectious disease services is simply a much larger financial and institutional lift in such contexts.
Even in countries with greater capacity, transition timelines should reflect country capacity, epidemiological realities, and progress toward disease control targets—not an arbitrary deadline imposed by Washington. For example, in the HIV context, countries nearing the 95-95-95 targets (i.e., 95% of people living with HIV know their status, 95% of them are on ARTs, and 95% of those on ARTs achieve viral suppression) may be well-positioned for accelerated transitions for that component of global health programming. However, countries struggling with high incidence rates, weak testing and treatment cascades, or emerging drug resistance require sustained support to avoid backsliding.
Further, success in one disease area shouldn't obscure broader health system needs. Transition decisions have to consider performance across multiple diseases and the core health infrastructure, not just individual program metrics. In that regard, helping countries to transition to integrated government provision will take considerable technical support—something that is largely dismissed in the strategy. Looking at PEPFAR’s fiscal year 2024 expenditures, approximately 18 percent of total investments support what the strategy labels low-priority site-level technical assistance (everything beyond commodities, healthcare worker salaries, and other expenditures on direct service delivery). This includes data collection systems that track treatment adherence, quality assurance and quality improvement initiatives that prevent medical errors, training programs that help healthcare workers adopt new technologies and treatment protocols, and community outreach efforts that identify and link patients to care. The considerable majority of investment in this type of work—63 percent—directly enables lifesaving treatment programs. An additional 10 percent of total expenditures supported "above-site" systems strengthening efforts including health financing mechanisms, policy development, and health system infrastructures, that will be especially critical during rapid transitions toward integrated, recipient government-executed programming.
Strategy implementation will also require considerable capacity and flexibility within the US government itself. While the document promises "U.S. government staff presence on the ground where possible, with a larger number of staff dedicated to geographies with the highest risk," the current reality is notably different. The State Department has hired only 30 new overseas positions for global health oversight, compared to approximately 168 health foreign service officers who were working prior to January 20. Meanwhile, realizing synergies across disease and health areas will require not only technical assistance and capacity building in recipient countries, but also addressing a structural challenge within the US government: how to implement flexible, cross-cutting programs within nearly 100 percent earmarked appropriations.
Sunset deaths, not assistance
Beyond country transition timelines, capacity constraints, and integration complexities, the strategy is aimed toward the wrong endpoint. It discusses sunsetting U.S. financing, but the real goal should be sunsetting the need for US financing everywhere. As developing countries get richer, they should take on more of the burden of fighting disease like malaria and HIV. But imagine Malawi’s income per person grew at a rate of 7 percent a year from now—it would still take 36 years to get to South Africa’s GNI per capita. The way to speed transition isn’t to wait until Malawi has the capacity and income required to provide the services to fight these diseases today; it is to dramatically reduce the capacity and income required to successfully fight these diseases tomorrow. This is the sunset we should aim for: the end of malaria and HIV as major health threats worldwide.
We now have some of the tools to achieve this vision: malaria vaccines already rival some of the best buys in global health in terms of cost per life saved, and 19 countries have introduced them into their childhood vaccination programs. We have the potential to vaccinate all children at risk in the next couple of years and save over 800,000 children’s lives by 2030. Meanwhile, breakthrough HIV prevention technologies like lenacapavir can disrupt transmission chains. Clinical trials of lenacapavir show 96 to 100 percent efficacy at preventing HIV transmission with just two pills per year. Notably, lenacapavir is especially useful for people who struggle to stick to a routine of daily pills—like young men, where adherence has been found to be as low as 26 percent. In high prevalence settings, putting just 4 percent of the population on the drug might prevent 20 percent of new infections.
And HIV vaccines are on the horizon (with considerable research previously funded by the US). An Operation Warp Speed for highly effective, cheap-to-manufacture malaria and HIV vaccines would be game-changing. Such an effort would accelerate a trend already underway: making these diseases increasingly affordable to manage. Antiretroviral drug costs have dropped from $14,000 per person per year in 1990 to under $45 per person by 2023. This shift isn’t just about reducing the need for and cost of treatment, it’s about simplifying the infrastructure needed for coverage. Instead of requiring extensive high-capacity delivery systems for testing and daily drug delivery, vaccinations could operate within existing routine public health programs.
In turn, that would mean US financial support could fall alongside infection rates. It is beyond the scope of this blog to forecast the potential cost of making malaria and HIV control so cheap and regular that it no longer requires a dedicated aid-funded effort, but it’s an exercise well worth pursuing.
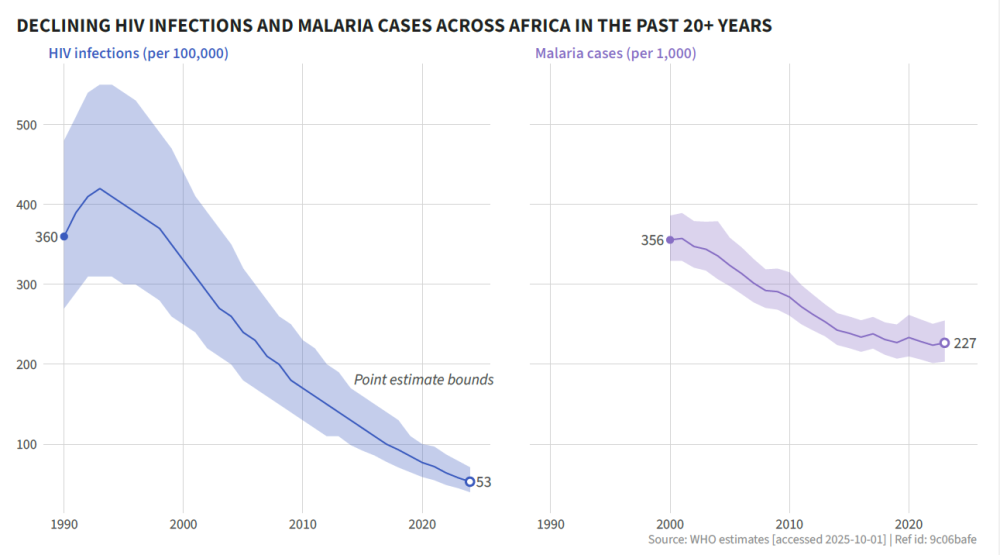
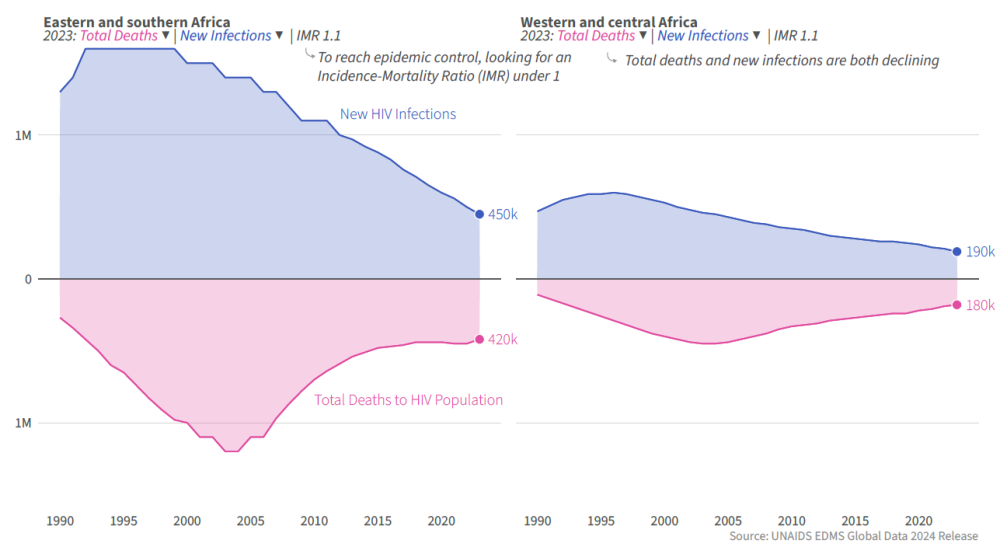
With US leadership through PEPFAR, the world has made amazing progress against a disease that—only a couple of decades ago—was a death sentence in much of the developing world. At its peak, about one in seven deaths in sub-Saharan Africa were caused by HIV/AIDS. It is now one in twenty. Since the launch of the US President’s Malaria Initiative in 2005, death rates from the disease in sub-Saharan Africa are down by a third. This is the time to double down, not walk away.
Americans have long supported the goal of making the world healthier—it is the most popular part of foreign assistance, with 83 percent of Americans backing it. In 1958, Eisenhower proclaimed in his State of the Union address that “we now have it within our power to eradicate from the face of the earth that age-old scourge of mankind: malaria.“ Referring to HIV in his State of the Union address in 2003, President George W. Bush promised the US would “ lead the world in sparing innocent people from a plague of nature.” President Obama’s 2016 State of the Union doubled down: “we’re on track to end the scourge of HIV/AIDS… and we have the chance to accomplish the same thing with malaria.” With advances in treatments, declining costs, and the wisdom to tailor transitions to country realities, this administration could deliver on what past administrations have only promised. It would be an impressive legacy.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.
Thumbnail image by: USAID in Africa/ Flickr








