Recommended
Eye health is having a moment.
Just last year, Bloomberg Philanthropies announced a $75 million Vision Initiative to expand access to screenings, eyeglasses, and cataract surgery across low- and middle-income countries (LMICs) and the United States. This is a major commitment in a sector that has historically struggled to attract large-scale funding. At the same time, at the UN General Assembly, the government of Antigua and Barbuda announced that it will host the first ever Global Summit on Eye Health in 2026.
For a field long relegated to the margins of global health and development, these are unusual—and encouraging—signals. But they also raise an obvious question for governments and for donors: why eye care, and why now?
Two new pieces of evidence—The $1 Trillion Blindspot and The Value of Vision investment case—help formalize what some governments and stakeholders have been stating for years: that vision loss is more than a health issue. It is a drag on multiple development outcomes including productivity, learning, road safety, and overall quality of life. They also show that much of this loss is avoidable with low-cost eyeglasses and cataract surgery, generating high returns on investment. (Disclosure: I serve as Chief Economist at the Seva Foundation, which led both pieces of work.)
A trillion-dollar development blind spot
A new analysis—The $1 Trillion Blindspot—goes beyond disability-adjusted life years (DALYs) to estimate productivity losses from uncorrected visual impairment in LMICs. Focusing on four streams of economic loss, the study finds that the productivity loss of visual impairment in LMICs is Int$ 1.1 trillion annually (Figure 1). This is equivalent to 1.2 percent of combined gross national income, more than the direct costs of natural disasters globally.
Figure 1. Productivity loss from visual impairment in LMICs
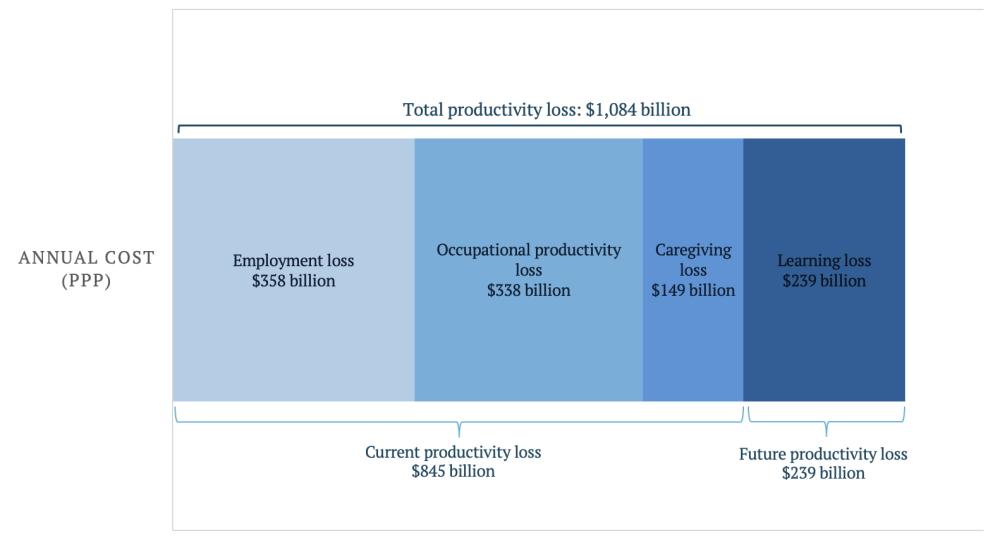
Source: Wong and Everett (2025).
The study draws upon the emerging evidence on the productivity, income, and learning effects from correcting vision in LMICs. These studies suggest, for example, that providing appropriate vision correction can raise productivity or income by 6 percent and 33 percent in specific settings, and that children with myopia learn half as much as children with good vision on average.
Given the enormous prevalence of uncorrected vision loss—1.1 billion people, 90 percent of which reside in LMICs, the economic impacts quickly add up to a substantial figure. Reframed this way, visual impairment is not just a health issue but also a productivity and growth problem.
Turning evidence into an investment case
If The $1 Trillion Blindspot quantifies the losses, The Value of Vision asks: what can we realistically do about it over the next five years, and what would it cost?
Developed by the Seva Foundation, The Fred Hollows Foundation and IAPB the Value of Vision is the most comprehensive assessment to date of the costs and benefits of scaling up a package of priority eye health interventions across LMICs.
The interventions include community and school-based vision screening with on-the-spot provision of reading glasses, expanded access to eye exams, increased cataract surgical capacity, measures to reduce demand side barriers, and improvements in surgical quality. Improvements in vision impairment are translated into a range of socio-economic benefits, including productivity gains, better learning and fewer road accidents. On the costing side, the model uses primary unit cost data from 55 eye-care providers in 29 LMICs.
Using a decision-tree framework, the report models realistic expansion paths of the intervention package across 111 LMICs from 2026 to 2030. The model shows that a US$7.1 billion investment in the interventions over five years could:
- Reduce vision impairment by around 24 percent by 2030, restoring clear sight to about 255 million people
- Deliver a raft of improved human development outcomes including 3.3 million additional equivalent years of schooling, 211,000 averted road injuries, and 1.7 million averted cases of depression
- Generate US$199 billion in productivity benefits over the same period—an average return of US$28 for every US$1 invested.
Large, measurable gains in human capital and development are achievable in eye care at a scale and cost that are modest relative to many other development priorities.
The evidence base underpinning these economic models is far from perfect. For example, there are only a handful of studies that directly measure the economic impact of correcting people’s vision. The PROSPER trial among tea pickers in India and the THRIVE trial among garment workers in Bangladesh report large productivity and income gains of 22 and 33 percent respectively. But these are relatively niche populations, so it is unclear how the findings generalize. Recent studies in other agricultural and manufacturing settings find more modest impacts of around 8 and 6 percent respectively—but these are still large enough to support high benefit–cost ratios.
What should governments and donors do?
Despite the remaining uncertainties in the evidence, many governments and donors are already moving to expand access to eye care. Research and implementation experience suggest a few clear policy levers to scale up the six interventions.
1. Fund and integrate eye care within universal health coverage
Eyecare has long been underfunded relative to its scale and economic cost. Closing that gap requires explicit budget lines in domestic health spending and in aid portfolios, and the inclusion of eyecare in national health benefit packages.
2. Demedicalize basic eye care
In many countries, basic eye screening and refraction are restricted to fully qualified optometrists, a cadre that is scarce and expensive to train. A more coherent approach is to demedicalize parts of vision care, enabling trained community health workers and mid-level eyecare personnel to provide screening and basic refraction with appropriate referral protocols. Moreover, providers should also be able to dispense ready-made reading glasses on the spot, as routinely happens in high-income countries. This frees specialists to focus on surgery and diagnosis of distance vision impairment and other eye pathologies.
3. Involve a broader suite of ministries, not just health
Because gains show up in productivity, employment, and education, countries with ambitious eye health agendas are typically driven by the executive and supported by multiple ministries. For example, prime ministers of Nepal and Antigua and Barbuda have championed eyecare, leading to greater prioritization across government. In Brazil, school eyecare programmes are financed jointly by the ministries of health and education. Similar cross-ministerial arrangements, including labour, transport, and social protection, can help align eye health investments with broader development strategies.
Taken together, the recent evidence on eyecare suggests that it merits a far more prominent place in debates about development, growth, and human capital. Few areas combine such a large underlying problem with interventions that are as tractable and cost-effective. At present, LMICs are effectively leaving $1 trillion in productivity on the table each year by underinvesting in basic eyecare. As the sector moves towards its first international summit in 2026, the next few years will be an important test of whether governments and donors are prepared to start capturing the returns that better vision can deliver.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.
Thumbnail image by: wirojsid/ Adobe Stock








