Recommended
The recent launch of the Global Compact for Nutrition Integration at the 2025 Nutrition for Growth Summit signaled renewed political commitment to addressing long-standing fragmentation in the delivery of nutrition interventions. It comes at a pivotal moment as health and development financing are at an inflection point. With highly constrained budgets and growing demands on health systems, there is widespread recognition that delivering nutrition services “as usual” is no longer viable. If nutrition investments are to be sustained and scaled up, they must align with broader efforts to deliver primary health care and with government priorities.
While awareness of the value of nutrition investments is growing, how these investments are financed and delivered within health systems has received less attention. We’re pleased to share a new CGD policy paper that takes stock of how nutrition interventions are currently delivered—and why that needs to change. It explores “diagonal” approaches as an alternative to vertical and horizontal models and offers policy recommendations for donors and governments to scale up the delivery of high-impact nutrition services.
The current landscape of nutrition service delivery
Delivery approaches for nutrition-specific interventions are characterized by three challenges:
1. Nutrition is often underprioritized, siloed, and poorly integrated into health systems and UHC efforts
Nutrition, health, and universal health coverage (UHC) are interconnected. Achieving good nutrition outcomes depends on strong health systems—and no country can reach UHC goals without integrating essential nutrition interventions across the life course. Yet in practice, nutrition is often treated as an “add-on” to service delivery or simply viewed as a broader determinant of health, rather than as a core set of preventive and therapeutic services that deserve direct investment via the health system.
This disconnect is reflected in government spending: Nutrition accounts for just 0.2 to 5.2 percent of total health spending in low- and lower-middle-income countries—significantly less than spending on infectious diseases and other conditions. As a result, a high coverage of general health services does not necessarily ensure adequate delivery of nutrition-specific interventions within the health sector.
2. Vertical approaches to nutrition-specific interventions often rely on off-budget funding, leading to parallel delivery systems
Nutrition-specific interventions tend to be delivered through vertical programs funded by external donors, although some donors, such as the World Bank—the largest funder—do channel a significant share of nutrition support on-budget (see Figure 1). These programs typically operate outside government budgets and via parallel systems, and are often managed by NGOs, private partners, or research institutions. This off-budget support has helped fill critical gaps and can achieve short-term wins through targeted and measurable outcomes. However, it frequently results in siloed delivery, duplicated efforts, and parallel supply chains, which often limit country ownership and create inefficiencies. This setup makes it harder for governments to coordinate, plan, or sustainably finance nutrition services.
Figure 1. Official development assistance for “basic nutrition” disbursement, 2020–22, by top donor and channel type
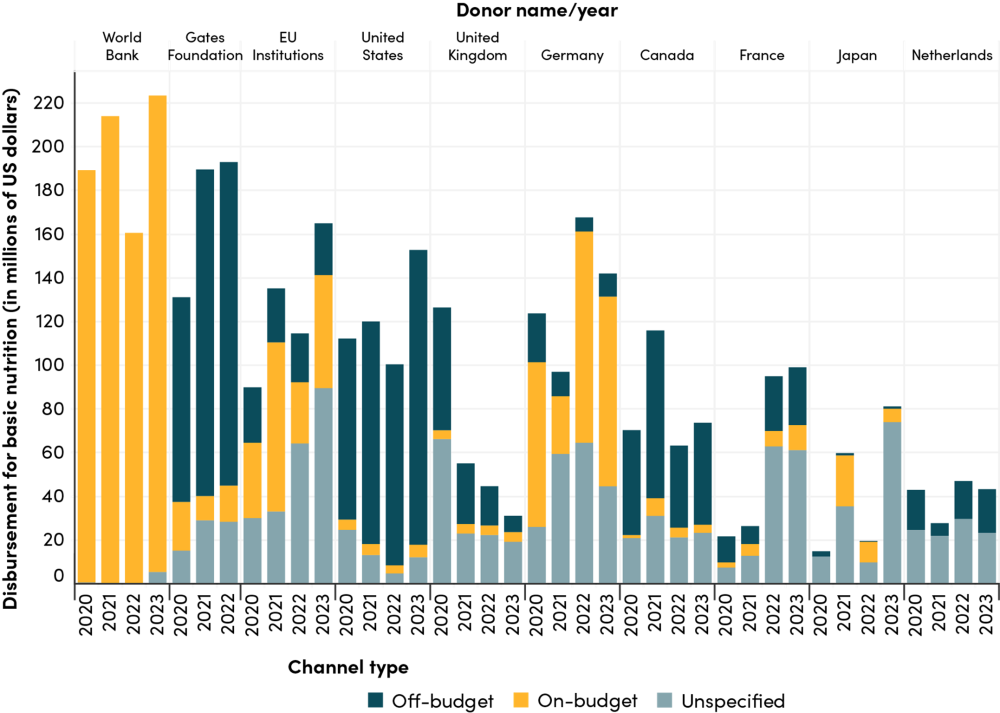
Source: Authors’ analysis of 2020-2022 data for “Basic nutrition” purpose code (12240), OECD Creditor Reporting System, accessed January 28, 2025.
Note: Data are filtered using the OECD CRS purpose codes “Basic nutrition.” The disbursement channels are defined as on-budget (governments, development banks), off-budget (NGOs, private sector, research), and unspecified (UN, others).
3. Horizontal approaches, while often on budget, make it hard to assess the impact on specific outcomes
Unlike vertical programs, horizontal approaches aim to support key health system components, such as improving infrastructure, workforce, and service delivery platforms. These investments are often more sustainable and tend to be on-budget, meaning they are channeled through government systems with higher country ownership and better aligned with national priorities. But they also come with tradeoffs: in low-resource settings, limited funds must cover many priorities, and without clear accountability mechanisms, it's hard to track results or ensure that nutrition-specific needs are adequately addressed.
Diagonal approaches could help bridge the dichotomy
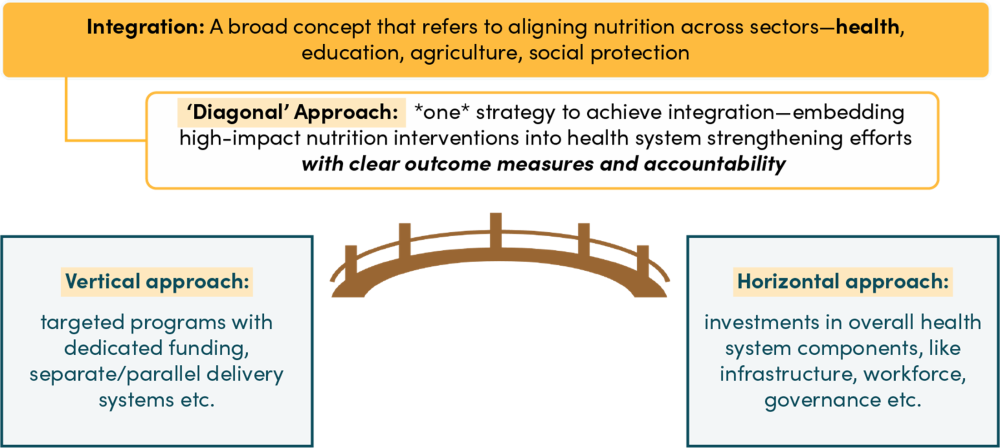
First introduced in Mexico’s 2006 health reform to reduce child mortality, diagonal approaches seek to embed high-impact nutrition interventions within broader efforts to strengthen health systems. Unlike purely vertical or horizontal models, this approach aims to achieve targeted outcomes and system improvements simultaneously. At its core, the diagonal approach emphasizes clear accountability and measurable results.
By focusing on cost-effective interventions with strong outcome tracking, diagonal approaches can help align donor priorities with domestic systems, while avoiding the inefficiencies of fragmentation. While this approach has been applied in areas like HIV and chronic disease, it is relatively underexplored in the nutrition space, and the limited available evidence is still mixed. However, it offers an alternative way forward to balance a focus on accountability while more firmly embedding nutrition interventions into health systems to achieve scale (see Figure 2).
Figure 2. Concepts of service delivery approaches
Why now?
With constrained budgets, rising health needs, and growing global attention on integration, the status quo for delivering nutrition services is being challenged. Translating high-level commitments into action—especially following the launch of the Global Compact of Nutrition Integration—can help optimize resources, strengthen accountability, and improve both nutrition outcomes and health systems. In this moment of fiscal pressure and reform momentum, diagonal approaches offer a timely and practical path forward.
Policy recommendations
Key message 1: Funders could benefit from understanding when and how to integrate
Donors can gradually shift toward diagonal integration by leveraging natural overlaps across three key areas: population targets, health system resources, and service delivery platforms. Progress can be further advanced by aligning financing mechanisms—either by channeling funds through government systems (on-budget) or by better coordinating off-budget approaches to reduce fragmentation and enhance sustainability (see Table 1).
Table 1. Diagonal approach models for nutrition integration
| Model | Integration approach | Illustrative examples |
|---|---|---|
| Overlaps in population targets | Combines nutrition interventions with existing health services based on life stages (e.g., child, maternal) | - Children: Vitamin A supplementation provided with routine immunizations and growth monitoring - Pregnant women: Multiple micronutrient supplementation (MMS) integrated into antenatal care (ANC) visits |
Overlaps in resources (health system components) | Utilizes shared infrastructure, workforce, and information systems to streamline operations | - Community health workers: Reach of nutrition programs expanded without separate distribution channels |
Overlaps in service delivery (preventive and primary care services) | Aligns nutrition counseling and education with preventive health care visits | - Primary care visits: Nutrition counseling on breastfeeding provided along with complementary feeding - Maternal and child health programs: Preventive nutrition education integrated into ANC and postnatal care |
| Overlaps in financing vehicles | Aligns donor and domestic funds to create sustainable, harmonized financing for nutrition within health systems | - Nutrition covered by national insurance - Matching fund arrangements: Donor and local funds combined |
Key message 2: Governments could facilitate integration by strengthening enabling factors
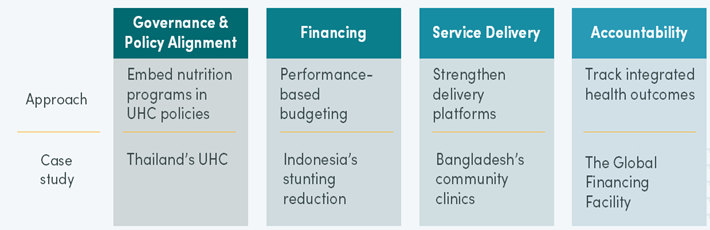
Making diagonal integration work requires coordinated action across multiple policy levers—including legislation, financing, and regulatory systems that influence how services are governed and delivered. While each country’s approach will vary, governments play a central role in enabling integration by strengthening four key areas: aligning policies and governance, creating financing models that reward integration, leveraging service delivery platforms, and building systems for monitoring and accountability (see Figure 3).
Figure 3. Enabling factors implementing the diagonal approach
The way forward
The global nutrition community faces a dual challenge: persistent undernutrition on one hand, and growing fiscal pressure and declining health coverage on the other. Although both vertical and horizontal approaches have demonstrated value, a move beyond this dichotomy through diagonal approaches offers a more sustainable path forward.
Looking ahead, several priorities emerge:
- Position nutrition at the heart of UHC reforms by aligning goals, financing, and delivery mechanisms.
- Strengthen the evidence base through better evaluation frameworks that capture both system-wide improvements and nutrition-specific outcomes.
- Enhance coordination and accountability by aligning donor and government efforts to reduce fragmentation and improve sustainability.
The recent 2025 Nutrition for Growth Summit created vital momentum for these shifts. Now is the time to move from commitment to operationalization and implementation—and reimagine how we deliver essential nutrition services within stronger, more resilient health systems.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.
Thumbnail image by: Dash/ Adobe Stock








